

100 Most Influential OT Research Articles
- Post date --> January 4, 2024
- Sticky post
Learn how we review the most influential occupational therapy research. And, see our 2024 list of the most influential OT-related journal articles.

How OT Potential helps you keep up with new research
Approximately 1,000 research articles containing OT are published EACH YEAR. That means roughly 5,000 articles have come out over the past five years!
As busy clinicians, we obviously don’t have time to keep up on all of the evidence. But, we do owe it to our patients to stay on top of the most influential research.
In our membership community, The OT Potential Club , we find and review the most influential research for you. In our two week rotation, we first share a written review of the research and give you space to discuss it. Then the follow week, we release an episode of the OT Potential Podcast , where we invite an expert guest to help us pull out actionable takeaways. These episodes are AOTA approved courses.
See the process in the video below. You can also sign up for a free trial to see our platform !
See sample journal article reviews and take 2 free CEU courses Sign up for our OT Potential Club free 5-day trial.
How we select OT research to review
Each year to determine the most influential research for us to review we generated a list the 100 most influential OT-related journal articles from the past 5 yeras.
We team up with a research librarian to make this happen.
For our 2024 list, we searched the Scopus database for articles published from 2019-2023 that had “ occupational therapy ” included in either the title, abstract, or keywords. (By the way, Elsevier’s Scopus is the largest abstract and citation database of peer-reviewed literature.) Then, we ranked the list by the number of times the articles had been cited in other journal articles.
The articles with green check marks have already been discussed in the OT Potential Club , and we will continue to work through this list throughout 2024.
To see research we’ve reviewed from past years’ lists check our article, research in the OT Potential Club .
The 100 most cited OT articles from the past five years
✅ = already reviewed in the ot potential club and featured as ceu course on the ot potential podcast.
- Listen to the podcast: Parkinson Disease Evidence Review with Brandy Archie
- Listen to the podcast: Cerebral Palsy and OT Evidence with Iona Novak
- Listen to the podcast: Rheumatoid Arthritis and OT with Cheryl Crow
- Listen to the podcast: OT and Psoriatic Arthritis with Duana Russell-Thomas
- Spinocerebellar ataxia (2019) Nature Reviews Disease Primers
- Considering the potential for an increase in chronic pain after the COVID-19 pandemic (2020) Pain
- Occupational Therapy Practice Framework: Domain and Process-Fourth Edition (2020) American Journal of Occupational Therapy
- American College of Rheumatology/Arthritis Foundation Guideline for the Treatment of Juvenile Idiopathic Arthritis (2019) Arthritis Care and Research
- Outpatient Physical, Occupational, and Speech Therapy Synchronous Telemedicine; A Survey Study of Patient Satisfaction with Virtual Visits during the COVID-19 Pandemic (2020) American Journal of Physical Medicine and Rehabilitation
- Secondary Fracture Prevention: Consensus Clinical Recommendations from a Multistakeholder Coalition (2020) Journal of Bone and Mineral Research
- Long-Term Effects of Breast Cancer Surgery, Treatment, and Survivor Care (2019) Journal of Midwifery and Women’s Health
- Cerebral palsy in children: A clinical overview (2020) Translational Pediatrics
- Listen to the podcast: Depression in Neurodegenerative Diseases with Rachel Wiley
- Listen to the podcast: Pediatric OT Evidence Review with Michelle DeJesus
- Pediatric Teleheath: Opportunities Created by the COVID-19 and Suggestions to Sustain Its Use to Support Families of Children with Disabilities (2021) Physical and Occupational Therapy in Pediatrics
- Listen to the podcast: Virtual Reality and OT with Christopher Gaskins
- Benefits of pulmonary rehabilitation in covid-19 – a prospective observational cohort study (2021) ERJ Open Res
- Emerging health challenges for children with physical disabilities and their parents during the COVID-19 pandemic: The ECHO French survey (2021) Annals of Physical and Rehabilitation Medicine
- Cerebral palsy: An overview (2020) American Family Physician
- Complex regional pain syndrome: a narrative review for the practising clinician (2019) British Journal of Anaesthesia
- Social Isolation – The Other COVID-19 Threat in Nursing Homes (2020) JAMA – Journal of the American Medical Association
- Listen to the podcast: CIMT and OT with Catherine Hoyt
- Assessment of Emergency Department and Inpatient Use and Costs in Adult and Pediatric Functional Neurological Disorders (2021) JAMA Neurology
- Canadian guideline for Parkinson disease (2019) CMAJ
- A systematic review of ayres sensory integration intervention for children with autism (2019) Autism Research
- Professional identity: A concept analysis (2020) Nursing Forum
- Sepsis-associated encephalopathy and septic encephalitis (2021) Expert Review of Anti-Infective Therapy
- Diagnosis and management of functional neurological disorder (2022) BMJ
- Listen to the podcast: OT for Spasticity in Adults with Scott Thompson
- Elements virtual rehabilitation improves motor, cognitive, and functional outcomes in adult stroke (2019) Journal of NeuroEngineering and Rehabilitation
- Clinical Neurorestorative Therapeutic Guidelines for Spinal Cord Injury (2020) Journal of Orthopaedic Translation
- Immersive Virtual Reality Mirror Therapy for Upper Limb Recovery after Stroke: A Pilot Study (2019) American Journal of Physical Medicine and Rehabilitation
- Best-evidence for the rehabilitation of chronic pain part 1: Pediatric pain (2019) Journal of Clinical Medicine
- Developmental delay: Identification and management at primary care level (2019) Singapore Medical Journal
- Listen to the podcast: OT and Functional Neurological Disorder
- One year in review 2019: Systemic sclerosis (2019) Clinical and Experimental Rheumatology
- Personalized medicine for patients with COPD: Where are we? (2019) International Journal of COPD
- Association of Geriatric Comanagement and 90-Day Postoperative Mortality among Patients Aged 75 Years and Older with Cancer (2020) JAMA Network Open
- Immersive Virtual Reality for the Management of Pain in Community-Dwelling Older Adults (2019) OTJR Occupation, Participation and Health
- Nonpharmacological Interventions to Improve Depression, Anxiety, and Quality of Life (QoL) in People With Dementia (2020) Journal of Geriatric Psychiatry and Neurology
- Occupational therapy for people with dementia and their family carers provided at home (2019) BMJ Open
- Decade of progress in motor functional neurological disorder: Continuing the momentum (2021) Journal of Neurology, Neurosurgery and Psychiatry
- Management of Osteogenesis Imperfecta (2020) Frontiers in Endocrinology
- Multiple sclerosis management during the COVID-19 pandemic (2020) Multiple Sclerosis Journal
- Parent perspectives of an occupational therapy telehealth intervention (2019) International Journal of Telerehabilitation
- Breast cancer in adolescent and young adult women under the age of 40 years (2021) JCO oncology practice
- Effects of telerehabilitation in occupational therapy practice: A systematic review (2019) Hong Kong Journal of Occupational Therapy
- Awareness and current knowledge of Parkinson’s disease: a neurodegenerative disorder (2019) International Journal of Neuroscience
- Cognitive reserve and age predict cognitive recovery after mild to severe traumatic brain injury (2019) Journal of Neurotrauma
- Cognitive training for people with mild to moderate dementia (2019) Cochrane Database of Systematic Reviews
- Physical Rehabilitation in Critically Ill Children: A Multicenter Point Prevalence Study in the United States (2020) Critical Care Medicine
- Quality of life and its related factors for adults with autism spectrum disorder (2019) Disability and Rehabilitation
- Extracorporeal Membrane Oxygenation Is a Team Sport: Institutional Survival Benefits of a Formalized ECMO Team (2019) Journal of Cardiothoracic and Vascular Anesthesia
- Motor learning in neurological rehabilitation (2021) Disability and rehabilitation
- Guidelines on the diagnosis and management of the progressive ataxias (2019) Orphanet Journal of Rare Diseases
- Construct validity, test-retest reliability, and the ability to detect change of the Canadian Occupational Performance Measure in a spinal cord injury population (2019) Spinal cord series and cases
- Telerehabilitation During the COVID-19 Pandemic in Outpatient Rehabilitation Settings (2021) Physical Therapy
- Loss in services precedes high school exit for teens with autism spectrum disorder (2019) Autism Research
- Construct validity of a revised version of the Occupational Balance Questionnaire (2020) Scandinavian Journal of Occupational Therapy
- Telehealth for the provision of occupational therapy: Reflections on experiences during the COVID-19 pandemic (2020) International Journal of Telerehabilitation
- Treatment patterns in children with autism in the United States (2019) Autism Research
- Stroke self-management and the role of self-efficacy (2021) Disability and rehabilitation
- Occupational therapy in the promotion of health and well-being (2020) The American Journal of Occupational Therapy
- Toward a theory-based specification of non-pharmacological treatments in aging and dementia (2020) Alzheimer’s & Dementia
- Efficacy of Virtual Reality Combined With Real Instrument Training for Patients With Stroke: A Randomized Controlled Trial (2019) Archives of Physical Medicine and Rehabilitation
- Relationships between job satisfaction, burnout, professional identity and meaningfulness of work activities for occupational therapists working in mental health (2019) Australian Occupational Therapy Journal
- Potential benefits of music playing in stroke upper limb motor rehabilitation (2020) Neuroscience and Biobehavioral Reviews
- Evaluation of pelvis postural systems in spinal cord injury patients: Outcome research (2020) Journal of Spinal Cord Medicine
- A review of interprofessional training wards: Enhancing student learning and patient outcomes (2019) Medical Teacher
- Effects of virtual reality-based planar motion exercises on upper extremity function, range of motion, and health-related quality of life (2019) Journal of neuroengineering and rehabilitation
- What is the threshold dose of upper limb training for children with cerebral palsy to improve function? A systematic review (2020) Australian occupational therapy journal
- Listen to the podcast: OT, Plagiocephaly, and Cognitive Outcomes with Amirra Condelee
- COVID-19 and Cerebrovascular Diseases: A Systematic Review and Perspectives for Stroke Management (2020) Frontiers in Neurology
- The use of augmented reality for rehabilitation after stroke: a narrative review (2020) Disability and rehabilitation. Assistive technology
- Listen to the podcast: Pain and OT with Irvin Eisenberg
- Flexor tendon rehabilitation in the 21st century: A systematic review (2019) Journal of Hand Therapy
- An intervention to reduce neuropsychiatric symptoms and caregiver burden in dementia: Preliminary results from a randomized trial of the tailored activity program–outpatient version (2019) International Journal of Geriatric Psychiatry
- Pharmacological and non-pharmacological therapeutic strategies in difficult-to-treat rheumatoid arthritis: A systematic literature review informing the EULAR recommendations for the management of difficult-to-treat rheumatoid arthritis (2021) RMD open
- Patient satisfaction with telehealth in rural settings: A systematic review (2020) International journal of telerehabilitation
- Physical, occupational, and speech therapy for children with cerebral palsy (2020) Developmental medicine and child neurology
- Enhanced recovery after surgery trends in adult spine surgery: A systematic review (2020) International journal of spine surgery
- Impact of Sarcopenia on Adverse Outcomes after Allogeneic Hematopoietic Cell Transplantation (2019) Journal of the National Cancer Institute
- Optimal Terminology for Services in the United States That Incorporate Horses to Benefit People: A Consensus Document (2021) Journal of alternative and complementary medicine
- Improving the quality of life of people with advanced respiratory disease and severe breathlessness (2019) Breathe
- Comparative efficacy of interventions for reducing symptoms of depression in people with dementia: Systematic review and network meta-analysis (2021) BMJ (Clinical research ed.)
- Listen to the podcast: OT & Smart Home Tech Adoption with Carol Chiang
- Contributing to social transformation through occupation: Experiences from a think tank (2019) Journal of Occupational Science
- Moving from cultural competence to cultural humility in occupational therapy: A paradigm shift (2020) The American journal of occupational therapy
- Virtual reality in neurorehabilitation: An umbrella review of meta-analyses (2021) Journal of clinical medicine
- Recommendations for the Nonpharmacological Treatment of Apathy in Brain Disorders (2020) The American journal of geriatric psychiatry
- Evidence-based practice implementation in stroke rehabilitation: A scoping review of barriers and facilitators (2020) The American journal of occupational therapy
- Treatment of neuropathic pain after peripheral nerve and brachial plexus traumatic injury (2019) Neurology India
- Cultural competency and the reproduction of White supremacy in occupational therapy education (2020) Health Education Journal
- Rural-urban disparities in health care costs and health service utilization following pediatric mild traumatic brain injury (2019) Health services research
- Listen to the podcast: OT and CRPS with Megan Doyle
- Interventions to improve upper limb function for children with bilateral cerebral palsy: a systematic review (2019) Developmental medicine and child neurology
- Re-imagining occupational therapy clients as communities: Presenting the community-centred practice framework (2019) Scandinavian journal of occupational therapy
- Occupational therapy, everyday life and the fabric of life: Theoretical-conceptual contributions for the construction of critical and emancipatory perspectives (2020) Cadernos Brasileiros de Terapia Ocupacional
- Hyperphosphatemic Tumoral Calcinosis: Pathogenesis, Clinical Presentation, and Challenges in Management (2020) Frontiers in Endocrinology
- Early versus delayed mobilization for in-hospital mortality and health-related quality of life among critically ill patients: A systematic review and meta-analysis (2019) Journal of intensive care
Need help accessing these articles?
As you can see, each of the articles in our list is hyperlinked for your convenience—and I’m always surprised by how many research articles are free! However, if you find one that is not free, you can also see if it’s available via your AOTA membership in AJOT or via ProQuest with your NBCOT membership. You can read more about these options in our blog post on where to find OT research .
All that being said, some articles you may simply have to purchase.
Resources derived from our OT research list
As we spend time exploring this research, we’ll continue to systematically pull information that is helpful for OTs. Check out these other blog posts, which incorporate information we find in our research:
- Helpful List of OT Journals
- List of OT Assessments
- OT Documentation
We hope this list fills you with excitement for occupational therapy—and the research that is driving it. And, we hope you consider joining us in our favorite corner of the internet…the OT Potential Club . 🙂
13 replies on “100 Most Influential OT Research Articles”
Thanks for taking the time to research and share these articles, I live by and truly believe that Team Work Makes a Dream Work! I look forward to our club and please count me in 🙂 One way that I would keep up with the latest and greatest was having mini lunch time discussions with my therapy pals. We would switch off who was responsible to bring in an article and share what we learned but most importantly how we can apply it. I think if more DOR could get behind these groups this would make big impacts in our daily practices. Look forward to your next blog! Aloha <3
Hey Monica!!
I am so excited to hangout with you in the OT Potential Club, and talk about ways to apply new research! I agree that lunch time journal clubs are such a great tool for departments. Hopefully the OT Potential Club will make preparing content for these even easier!
Thank you so much for all your support! (And please send some of your warm weather to those of us in the Midwest!)
As a future OT student, I’m curious if you have any insight into the following question. As I read about advancements in childhood development research, it strikes me that OT’s are often not included in these discussions. For instance, I went to a Brookings Institution panel on "A prescription for play" ( https://www.brookings.edu/blog/education-plus-development/2018/08/21/a-prescription-for-play/ ) and it would have been great to have an OT on the panel since they work "on the ground" with children. As neuroscience continues to break ground on new issues related to childhood development (i.e. the brain and trauma), why aren’t OT’s being included in these discussions? Is it because they are considered practitioners and not researchers?
Hi Laura, You’ve stumbled onto a huge problem here, and it isn’t specific to OT. One often cited study showed that it takes about 17 YEARS for new medical knowledge to be adopted into practice (and even then only a fraction of best practices actually get adopted.) There is clearly a disconnect between academia and practitioners on the ground. To solve the complex challenges of today and the future, we certainly need new tools and bridge builders to help us shorten this gap!
Thanks – this is helpful to know. And I’m glad it’s just a problem with OT, because it had me wondering what the issue was.
*it’s not just
Hi Laura. As Sarah stated, you’ve stumbled upon a huge problem, that I think IS specific to occupational therapy. The medical and research communities (and general community for that matter) remain under-educated about the existence and value of the occupational therapy profession. We very rarely have a seat at the table, as you recognized. Occupational therapy, though being around for over 100 years, continues to be quite insulated. Although this is changing! In my opinion, AOTA has never done an excellent job of marketing us OUTSIDE the occupational therapy community, and thus hasn’t had the skillset to teach us how to market ourselves. This is a challenge I continue to struggle with but am working solidly towards addressing.
A few strategies I use are to always identify myself as an "occupational therapist," instead of an "OT" and I work in the field of "occupational therapy". I also don’t refer to PT in my definition of what occupational therapy is. A third way I do this is to have an elevator pitch of what occupational therapy is ready at all times.
Hope this helps answer your question 🙂
Love, love, love this post and the list!! Ever an inspiration, Sarah!
Ahhh! Thank you! I am consistently inspired by the OT community and can’t wait to hang out with OT practitioners in the OT Potential Club!
I wish there were more exert articles about OT in Mental Health, such a great need for mental health supports now-a-days!
It’s awesome.. Am amazed. I was able to conduct my research problem.
Oh wow! I’m so glad to hear that! What was your research problem?
Thanks for sharing these articles, they are so useful. 🙂
Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.

Occupational Therapy : Research Proposal
- Research Proposal
- Discovery@RML
- E-Journals This link opens in a new window

Credit: IJRTOnline
Helpful handouts.
- Literature Review How-To
- Literature Review - Annotated Example
- Literature Search Tracking Log
- Literature Review Tracking Log
- Qualitative Data Collection
- Quantitative Data Collection
- Introduction
- Literature Review
- Research Design
- Methodology
The Introduction section of the research proposal should provide the reader with an overview of your research. You want to take the time to briefly explain why you selected your topic and why it is important to your field. You will then want to express what your research adds to the field and why it is important. It is helpful for the reader and yourself to use the section to define terms and/or concepts that will be important to your proposal and overall research. The introduction should conclude with your research question(s) or hypothesis(es) and what you aim to learn or achieve by completing this research. Many find it helpful to make the Introduction the last section that they complete. By doing this, you will have a clearer understanding of your overall research strategy and research question.
Your introduction should do the following:, explain the problem being investigated and related issues, explain the purpose of investigating the problem, provide relevant background or historical information , explain research trends and relevant theories for the field, define key terms and theories , set parameters and aims for the study, state the proposals research question(s) or hypothesis(es), the literature review section of your research proposal is where you present an analysis of the published literature on your research topic. the literature review does not need to cover every published paper or book but should survey scholarly literature that is the most important research within your field and on your particular topic. the goal of the literature review is to analyze the available body of literature and to present how it is related, either through theory, method, or concepts. you want to show the reader that your research fits any gaps present within the field, therefore making your research new and valuable to the field. , organize your results. , utilize literature review trackers , save all your journal articles to one place , keep track of databases searched and terms used. , group findings., you want to find similarities and differences in the literature. , try grouping by methods, concepts, theories, or findings., look for controversy., is there a debate within your field of study , are some researchers using one theory over another, find the gaps. , you want to find the gaps in the literature to help show that your research is new and important to the field. , do not summarize. , you want to ensure that you are analyzing the literature in your review, don't just summarize each study. .
The Research Design section of your research proposal is where you will explain your research plan and the process and procedures that will go into carrying out your plan.
You should explain the type of research you will be performing: qualitative, quantitative, mixed-methods, etc. this determination will impact all other components of your research plan from population to data analysis (pickard, 2013, 52-53)., this section should answer the following questions:, is your study qualitative, quantitative, or mixed-methods, why have you made this decision, why is this the most appropriate study design, qualitative.

Quantitative
The methodology section is where you describe exactly how you anticipate carrying out your research. this section will include detailed explanations of your research methods, data collection, and data analysis (pickard, 2013, 53). , you should be answering the following questions:, what research method(s) are you applying to the study, why have you made this choice, how do you intend to structure the method(s) for your investigation, population , you will first need to determine who will constitute your research population, i.e. who are you studying are you planning on studying a large group of people, or a small group. this decision will be in part be determined by your research design and methods. , "your research population is the entire set of individuals about which inference will be made." (pickard, 2013, 60). , sampling methods are used when you cannot include everyone in your research population, and therefore there is a need to create a pre-defined 'sample' of your population. within this section, you will need to explain how you plan on obtaining your sample and why this sampling method is the most appropriate and generalizable. , "sampling is the process of selecting a few from many in order to carry out empirical research." (pickard, 2013, 59). , types of sampling techniques:, probability sampling, simple random sampling, stratified random sampling, cluster sampling, quota sampling, purposive sampling, a priori criteria sampling, snowball sampling, data collection, within this section, you will need to explain who you plan to obtain your research data and what type of data you plan on collecting. will you be performing an experiment with data points, an interview with questions, or will you be utilizing a research instrument the research design and type of data will determine your data collection procedures. remember that data collection techniques are tied with data analysis, the type of procedure for data collection must match how your data will be analyzed. , examples of data collection techniques:, empirical , research instruments, questionnaires, reliability: measures consistency, validity: does it measure what it's supposed to measure, observations, focus groups , data analysis, in this section, you will need to explain how you plan to analyze the data you collected. the type of data analysis is based upon the type of data collected and your research design. you will need to determine if your research is quantitative or qualitative, this will impact how you will analyze your data. quantitative data analysis involves statistical calculations and procedures, while qualitative does not. , quantitative analysis, frequency distribution, mann-whitney u test, rank order correlation, all parametric statistics, qualitative analysis, comprehending, synthesizing, re-contextualizing, the research ethics section is where you describe how you plan to uphold ethical considerations. all research involving human or animal participants need to abide by ethical standards. the types of ethical considerations and standards you must consider for your research plan will depend on the type of research design, population, sample, and data collected. , you must show you understand and acknowledge the ethical boundaries placed on your research plan. , the irb or institutional review board is a type of committee that applies research ethics by reviewing the methods proposed for research to ensure they are ethical. , federal regulations involving human subjects must be reviewed by an irb. the irb must approve or determine the project to be exempt prior to the start of any research activities. , you must submit your research for irb approval if it meets the following criteria:, you are utilizing human participants, your data collection is systematic and methodical, the goal of your research is to contribute to the generalizable scientific knowledge base of your discipline, informed consent , you will need to obtain informed consent from your study participants. informed consent is a document that study participants agree to sign acknowledging that they understand what they are agreeing to, what is being asked of them, the purpose of the research, how their information will be used and/or protected, and are aware of any danger to their body or mind. informed consent creates a mutual understanding between researchers and study participants., data ethics, anonymity : the study participants remain totally anonymous during and after the research activity., confidentiality : the identity of the participants will not be revealed when using any data provided by that participant..
References:
Pickard, A.J. (2013). Research Methods in Information (2nd ed.). Chicago, IL: ALA Neal-Schuman.
Revised with permission: Research Process and Scholarship Guide , National University Library
- << Previous: Research
- Next: Databases >>
- Last Updated: Jun 25, 2024 8:51 AM
- URL: https://umc.libguides.com/OT
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Sage Choice

Enablers and challenges to occupational therapists’ research engagement: A qualitative study
Laura di bona.
1 Engagement Manager/Occupational Therapist, Sheffield Health and Social Care NHS Foundation Trust, Sheffield, UK
2 Honorary Research Fellow, School of Health and Related Research, University of Sheffield, Sheffield, UK
Jennifer Wenborn
3 Senior Clinical Research Associate/Occupational Therapist, Division of Psychiatry, University College London, London, UK
4 Dementia Research Centre, Research and Development, North East London NHS Foundation Trust, London, UK
Becky Field
5 Research Associate/Occupational Therapist, School of Health and Related Research, University of Sheffield, Sheffield, UK
Sinéad M Hynes
6 Lecturer, School of Medicine, Nursing and Health Sciences, National University of Ireland, Galway, Ireland
Ritchard Ledgerd
7 Clinical Researcher/Occupational Therapist, Dementia Research Centre, North East London NHS Foundation Trust, London, UK
Gail Mountain
8 Professor of Health Services Research, School of Health and Related Research, University of Sheffield, Sheffield, UK
Tom Swinson
9 Senior Research Assistant, Dementia Research Centre, North East London NHS Foundation Trust, London, UK
Introduction
To develop occupational therapy’s evidence base and improve its clinical outcomes, occupational therapists must increase their research involvement. Barriers to research consumption and leadership are well documented, but those relating to delivering research interventions, less so. Yet, interventions need to be researched within practice to demonstrate their clinical effectiveness. This study aims to improve understanding of challenges and enablers experienced by occupational therapists who deliver interventions within research programmes.
Twenty-eight occupational therapists who participated in the Valuing Active Life in Dementia (VALID) research programme reported their experiences in five focus groups. Data were analysed thematically to identify key and subthemes.
Occupational therapists reported that overwhelming paperwork, use of videos, recruitment and introducing a new intervention challenged their research involvement, whereas support, protected time and a positive attitude enabled it. The impact of these challenges and enablers varied between therapists and organisations.
Challenges and enablers to research involvement can be identified but must be addressed within individual and organisational contexts. Multifaceted collective action to minimise challenges and maximise enablers can facilitate clinicians’ involvement in research. Using this approach should enable occupational therapists to increase their research involvement, thus demonstrating the clinical effectiveness of their interventions.
Developing research-active clinicians and organisations has become a National Health Service (NHS) priority because of their positive impact on both clinical outcomes and the United Kingdom (UK) economy ( Boaz et al., 2015 ; Department of Health (DH), 2006 ). For occupational therapists, incorporating research activity into their interventions and services is a requirement of their code of ethics and professional conduct ( College of Occupational Therapists, 2015 ). When asked, the majority of occupational therapists report that they wish to be involved in research, but find it hard to do so, thus most are not ‘research active’ ( Pighills et al., 2013 ; White et al., 2013 ). While this is the case, occupational therapists, alongside other allied health professionals in similar positions, risk being marginalised within healthcare delivery due to an inadequate evidence base ( Pain et al., 2015 ).
There are many ways in which occupational therapists can engage with research. This has been termed a ‘research continuum’, ranging from activities that all occupational therapists should be doing, such as reading research literature, at one end, to research leadership activities, for the minority, at the other ( Pighills et al., 2013 ). In England, the Department of Health’s five-year strategy for research and development, Best Research for Best Health ( DH, 2006 ) led to increased investment in research infrastructure and capacity building for clinicians at all stages of this continuum. This included establishing the Health Education England/National Institute for Health Research (NIHR) clinical academic pathway to increase research capacity and leadership, and collaborations for leadership in applied health research and care (CLAHRCs) to increase applied research and its implementation ( National Institute for Health Research, 2016a , 2016b ). However, some research roles, such as healthcare professionals delivering research interventions and being research participants themselves, have received less focus despite the importance of this role for successful intervention development and research implementation ( Hysong et al., 2013 ; Newall et al., 2009 ).
Occupational therapists have been integral to the success of a number of research studies by virtue of their role in delivering the interventions being investigated (for example Eriksson et al., 2013 ; Killaspy et al., 2015 ; Sturkenboom et al., 2014 ). The increasing research on occupational-therapist-delivered interventions is a real opportunity for the profession to extend its evidence base. However, there has been little consideration given to how to recruit and engage healthcare professionals as research participants and what might be the challenges and enablers to doing so ( Hysong et al., 2013 ; Newall et al., 2009 ). The Valuing Active Life in Dementia (VALID) research programme involves occupational therapists in intervention delivery and has investigated the challenges and enablers to their engagement.
The VALID research programme
The VALID research programme aims to develop and evaluate a community occupational therapy intervention for people living with mild to moderate dementia and their family carers: Community Occupational Therapy in Dementia–UK (COTiD-UK) ( Wenborn et al., 2016 ). The programme builds on research of an intervention, community occupational therapy in dementia (COTiD), developed and found to be clinically and cost effective in the Netherlands ( Graff et al., 2006 , 2007 , 2008 ). The VALID research programme follows the Medical Research Council’s framework for developing and evaluating complex interventions and as such consists of a number of phases, including a randomised controlled trial ( Medical Research Council, 2008 ). The research reported in this paper was conducted within the initial multisite ‘development’ phase of the research programme, which customised the intervention to the UK setting and tested its feasibility in practice.
This development phase involved occupational therapists participating in a number of research activities (detailed in Table 1 ). Firstly, occupational therapists were trained in the COTiD intervention, ( Graff et al., 2006 , 2007 ). Secondly, they delivered this intervention to people living with dementia and their family carers. In some sites this also involved occupational therapists recruiting research participants and seeking informed consent. Finally, occupational therapists provided data about their activities within, and experiences of, the VALID research study. This included video recording intervention sessions, completing questionnaires about their own skill acquisition, detailing the time and content of the occupational therapy sessions provided and participating in a focus group.
Occupational therapists’ research responsibilities.
| Activity | Tasks |
|---|---|
| COTiD intervention training | • Attend five days’ training |
| • Read additional training materials | |
| • Practice learning between sessions e.g. standardised assessments with volunteers (peers, students or service users) | |
| • Receive and reflect on written feedback from COTiD trainers about videoed sessions | |
| • Supervision from COTiD trainers (within VALID research team) | |
| • Peer supervision (frequency varied between sites) | |
| Recruiting people living with dementia and their family carers as research participants to receive COTiD intervention (not all occupational therapists did this – in some sites, designated research staff completed this) | • Identify potential participants |
| • Provide participant information sheets | |
| • Seek informed consent | |
| • Complete consent forms | |
| • Recruitment data management | |
| COTiD intervention delivery | Provide 10 × 1 hour person-centred COTiD sessions in peoples’ homes/ community settings |
| Data collection | • Video record intervention sessions |
| • Complete questionnaires about occupational therapists’ skill acquisition and transfer of knowledge into practice | |
| • Record date, duration and content of occupational therapy sessions | |
| • Discuss opinions in a focus group |
This paper reports findings of focus groups in which occupational therapists discuss their involvement in the VALID research study, specifically what challenged or enabled their involvement.
To improve understanding of the challenges and enablers experienced by occupational therapists who deliver an intervention within a research study.
Literature review: challenges and enablers to research participation
A number of studies have described the research challenges and enablers as experienced by occupational therapists internationally (for example Eriksson et al., 2013 in Sweden, Gutman, 2009 in the USA, Pighills et al., 2013 in Australia, White et al., 2013 in the UK). Also for other allied health professionals and nurses (for example Akerjordet et al., 2012 in Norway, McMaster et al., 2013 and Newall et al., 2009 in Australia). Three challenges to research involvement appear to be most frequently cited by occupational therapists and other healthcare professionals: lack of time, money and skills ( Akerjordet et al., 2012 ; Gutman, 2009 ; McMaster et al., 2013 ; Pighills et al., 2013 ). Conversely, two enablers of research involvement are also widely cited: providing support and positive attitudes towards research ( McMaster et al., 2013 ; Pain et al., 2015 ; Pighills et al., 2013 ; White et al., 2013 ). However, these studies have tended to focus on identifying general challenges and enablers to research engagement, often at unspecified stages of the research continuum.
In contrast, little has been documented about the experiences of healthcare professionals who get involved in delivering the intervention component of research. Only two, non-UK based, studies were identified: one of occupational therapists ( Eriksson et al., 2013 ), the other of nurses ( Newall et al., 2009 ), in both cases participating in randomised controlled trials. Both studies found that clinicians placed great value on taking part in research and that this motivation and the support of others acted as enablers to their participation. However, Eriksson et al. (2013) highlighted that a lack of time and/or experience and anxiety about skills were challenges to research participation. Both studies also identified that difficulties with research participant recruitment challenged their own involvement ( Eriksson et al., 2013 ; Newall et al., 2009 ). Healthcare professionals, therefore, appear to report similar challenges and enablers to research engagement regardless of their profession or type of engagement along the research continuum. However, how these factors interact or how they apply to healthcare professionals delivering interventions within research programmes is not yet sufficiently understood.
Qualitative methods were selected as they are most appropriate for understanding participants’ experiences of little understood topics ( Silverman, 2013 ), in this instance occupational therapists’ challenges and facilitators to research involvement. Qualitative methods can also facilitate deeper understanding of the contexts in which interventions will be delivered ( Vernooij-Dassena and Moniz-Cook, 2014 ). Focus groups were chosen, in preference to interviews, to enable opinions to be gathered from more people and enable them to explore and clarify their views in a supportive environment ( Kitzinger, 2000 ).
An indicative topic guide was developed by the research team aiming to elicit opinions on three topics; firstly, how the COTiD intervention should be adapted for the UK context; secondly, the most and least effective elements of the training provided for delivering the intervention; and thirdly, enablers and challenges to research participation. Data about the first two topics informed the development of the COTiD-UK intervention and training and will be reported separately. Data collected in relation to the last topic were used when planning the next phases of the VALID research programme and are reported here.
Recruitment
Ten English healthcare organisations participated in the development phase of the VALID research programme, which included these focus groups ( Wenborn et al., 2016 ). Each organisation was asked to identify occupational therapists who could participate in the study. Forty-four occupational therapists participated, and all met the eligibility criteria of being registered as an occupational therapist with the Health and Care Professions Council, with experience of working in the community and/or with people living with dementia and their family carers. All were invited to attend a focus group after they had completed the COTiD training and delivered the intervention.
Ethical issues
The study was approved by the Yorkshire and the Humber – Leeds West National Health Service (NHS) Ethics Committee (reference number 12/YH/0492) on 16 November 2012. The study was also granted NHS research and development approval (reference number 13762). Occupational therapists provided signed informed consent. Data were anonymised and stored securely following usual data management procedures.
Participants
Twenty-eight (64%) occupational therapists from eight (80%) of the participating healthcare organisations took part in focus groups, with between two and eight occupational therapists representing each organisation. Twenty-six (93%) were women. Seven (25%) were band five (junior occupational therapists, 13 (46%) band six (specialist occupational therapist), six (21%) band seven (highly specialist occupational therapist) and two (7%) band eight (lead occupational therapist).
Data collection
Five focus groups were conducted with between five and eight occupational therapists attending each. Four members of the research team facilitated the focus groups, two facilitating each, with the exception of one smaller group with just three attendees that was facilitated by one person. The groups were audio recorded. Facilitators completed observational notes and reflexive analysis during and immediately following focus groups to document additional key information, such as participants’ facial expressions, gestures and researchers’ thoughts and interpretations. Audio recordings were independently transcribed verbatim and anonymised. Transcripts were checked for accuracy and missing data by focus group facilitators. As it was not possible to identify all focus group participants from the recorded transcript, each was identified only as a facilitator or participant.
Data analysis
Thematic analysis was carried out ( Guest et al., 2012 ). This involved each researcher reading one or two transcripts, ascribing codes, categories and then themes to the data. The research team discussed and iteratively checked these against the transcripts, looking for evidence of themes, categories and codes being confirmed or disconfirmed, to ensure trustworthiness and credibility ( Mays and Pope, 2000 ). Once there was agreement on the overall themes, categories and codes were then reapplied to the transcripts.
Two main themes emerged describing occupational therapists’ ‘research challenges’ and ‘research enablers’, each with four subthemes. See Figure 1 for details.

Occupational therapists’ research engagement: challenges and enablers.
Research challenges
Within the theme of research challenges, four subthemes were identified: ‘overwhelming paperwork’, ‘videos’, ‘recruitment’ and ‘delivering a new intervention’. These topics were raised by participants in all focus groups.
Overwhelming paperwork
There was a general consensus that research involvement had led to engagement in a range of additional administration and reporting tasks. For some, paperwork and emails presented a real challenge both in terms of volume and because these were updated during the course of their involvement. One therapist stated:
I have felt so overwhelmed, I have actually just dumped the whole lot and done nothing. I am just so confused and all the changes … (Focus group 2 participant).
However, whilet many appeared to agree with this sentiment, for others, additional administrative tasks were accepted as an essential, if time consuming, part of the research process.
The occupational therapists were required to video record the intervention sessions and then transfer the videos to the research team via an encrypted USB memory stick. Many described this as challenging, although different aspects were raised in different focus groups. Firstly, some had never used video recorders before, so had to learn this new skill, which not everyone found easy. Secondly, the quality of the video recorders was criticised for having limited battery life and being difficult to position in order to get all three participants in view (person living with dementia, carer and occupational therapist). One therapist, who had encountered many challenges, stated:
We spent countless, I cannot tell you how many frustrating countless hours with these video recorders that don’t video, that don’t charge, that don’t do this (Focus group 4 participant).
Thirdly, the impact of the cameras on rapport building was viewed by some as a good ice-breaker but more often they were viewed negatively. For instance:
When the camera goes off as well … everything comes out (Focus group 4 participant).
A number of occupational therapists described this phenomena of ‘opening up’ when cameras had been switched off, as this was usually when the therapist was due to leave, resulting in increased time pressures as they stayed to listen to what people had held back from saying on camera. Finally, therapists described difficulties in transferring videos from the camera on to computers to view them and then onto USB memory sticks to send to the research team. In some cases, this was because of a lack of familiarity and skills with the technology, in other cases because their organisations required special permission to enable them to use the software provided or had inadequate hardware.
Three recruitment-related challenges were reported. Firstly, those responsible for recruiting people living with dementia and their family carer to receive the COTiD intervention stated this was time consuming and required additional paperwork to be completed.
Recruitment … there was a lot of phone calls and visits before you actually get someone to say yes please … so juggling that with everything else (Focus group 3 participant).
Secondly, the plan of having service users recruited in readiness for occupational therapists to start working with alongside attending the COTiD training did not work out for a variety of reasons across the organisations. This meant that some therapists had a delay between completing their COTiD training and having service users ready to work with. One therapist summed up the difficulties this caused:
I suspect if I had done the couple straight away … I would have remembered a bit more … been a bit more enthusiastic (Focus group 5 participant).
Finally, some therapists reported that the service users recruited were not appropriate for the intervention, making it harder to deliver. For instance, stating they had volunteered altruistically for the study rather than because they wanted or were appropriate to engage with the intervention.
Delivering a new intervention
Occupational therapists had to learn to deliver a new intervention, COTiD. They expressed inconsistent, different opinions on the intervention aims and design; for example, whether or not it had the right amount of structure, was the right length or was person-centred enough. However, the majority appeared to appreciate working in an occupational therapy profession-specific way, for example:
It really does give you an opportunity to go back to the core of OT and spend some quality time (Focus group 3 participants).
For most, working in ways that were different to routine practice was challenging:
With the way memory services work we go in with a plan and we do it and we go out so this has been quite difficult to take a step back (Focus group 5 participant).
For some, the necessary level of scrutiny of their work to meet the research protocol requirements was also quite challenging:
Well I felt I was going to get slated as soon as that film went to someone to watch … you’re in the fear of have you done wrong (Focus group 4 participant).
Research enablers
Within the theme of research enablers were four subthemes, ‘peer support’, ‘management support’, ‘protected time’ and ‘positive attitudes towards research’. Each subtheme was identified in every focus group, with occupational therapy participants initiating discussion of the topic.
Peer support
All occupational therapists participated in peer support groups where they shared their experiences of participating in VALID, most also supported each other outside of these groups. They described three mechanisms by which this support enabled their research involvement. Firstly, by creating a safe environment for occupational therapists to practise clinical skills, such as standardised interviews, which they might not otherwise be using in day to day practice. Secondly, it enabled them to share feelings about research involvement and its challenges. Finally, it was useful to clarify quickly the required research procedures. For instance:
… somewhere to ask questions, like oh my goodness what do I do with this one rather than me ringing XX (lead researcher) (Focus group 1 participant).
While all who expressed an opinion described peer support as a positive enabler of research involvement, practical challenges to ensuring it happened were identified. Firstly, if there were not many occupational therapists within a geographical location, they either had to travel a long way for peer supervision or have it with such a small group that there were fewer experiences, views and expertise to be shared. However, if there were more therapists involved, finding a mutually convenient time and location to meet was difficult.
Management support
Occupational therapists reported differing experiences of management support. While all had management permission to engage in the study, some described additional mechanisms by which managers had facilitated their research involvement. Firstly, by championing VALID within their organisation, highlighting its importance to other colleagues and managers and encouraging occupational therapists to prioritise it within their workload. Secondly, by negotiating specific time, such as a day or two a week away from their usual role to focus solely on VALID. Finally, linking therapists with their research and development departments, who had subsequently provided further support, for instance with recruitment of participants and using the video cameras and associated software and hardware. One occupational therapist stated:
We couldn’t have done it without xx our OT (lead)… the amount of work that she has done (Focus group 3 participant).
In contrast to these positive experiences, some participants described having multiple managers with differing levels of enthusiasm and support for the research. Where support was more ambivalent, research involvement became more challenging. One occupational therapist stated:
Managers need to be on board… it was as if I was going off doing my own thing having a good time (Focus group 2 participant).
Occupational therapists, therefore, described how management support enabled research involvement in multifaceted ways, but highlighted that they often had more than one manager and it was easier when all were actively supportive.
Protected time
All occupational therapists who expressed an opinion stated that having protected, funded time, to focus solely on VALID was a major enabler of research involvement. In contrast, those participating in VALID without allowances made for their usual roles, described it causing tension within teams, as they were less available for other work. One therapist described it as ‘balancing two jobs’ [Focus group 1 participant], and some described feeling that this compromised the quality of both their clinical and research work. Most of those without protected time reported completing much of their research paperwork, intervention preparation and sometimes even the intervention, in their own time. Generally, risk management, crisis and generic work took priority. For instance:
By the time I got back to the office and you’ve got a semi crisis on VALID’s gone out the window (Focus group 4 participant).
In contrast, the minority who had protected time, such as 1 or 2 days a week focusing solely on VALID, did not describe the same difficulties.
Positive attitudes towards research
Occupational therapists mostly expressed positive attitudes towards research involvement. Some spoke with great enthusiasm about how participating in research had given them the opportunity to deliver an intervention they valued. COTiD was described positively by many as being ‘core OT’ and by some as person-centred and less time pressurised than much of their other work. One participant stated:
I was having this discussion with my manager, he said to me, ‘what is different?’ and I said ‘what is different is the quality’ (Focus group 3 participant).
For others, it was involvement in the research process itself that they valued, describing benefits for themselves as increasing their research understanding, capacity and experience. Some felt that by participating in VALID they were contributing to the development of the occupational therapy profession on a local and national level.
On a local level it’s very exciting for us to have this research to try and raise the profile of OT so you know I think it’s a fantastic opportunity to be part of it (Focus group 5 participant).
Occupational therapists reported that overwhelming paperwork, use of videos, recruitment and introducing a new intervention challenged their research involvement, whereas support, protected time and positive attitudes enabled it. These enablers and challenges broadly concur with those identified in previous studies of clinicians’ participation in randomised controlled trials ( Eriksson et al., 2013 ; Newall et al., 2009 ). They are also similar to those identified at other stages of the research continuum, such as implementing evidence-based practice and research leadership development ( Akerjordet et al., 2012 ; Gutman 2009 ; McMaster et al., 2013 ; Pain et al., 2015 ; Pighills et al., 2013 ; White et al., 2013 ).
Implementing a research study within clinical practice was found to be a complex, multistage process. While there were commonalities in the research challenges and enablers identified by occupational therapists, the degree of their impact varied. This is consistent with understandings from implementation science that individual and organisational contexts are hugely influential, to the extent that what one person considers a challenge, another may consider an enabler ( Damschroder et al., 2009 ; May et al., 2016 ). Normalisation process theory helps explain how new practices are operationalised in healthcare and other settings ( May and Finch, 2009 ). It describes four mechanisms through which changes to practice are implemented ( May and Finch, 2009 ):
- coherence (sense making and meaning);
- cognitive participation (personal engagement);
- collective action (organisational engagement and interaction to implement);
- reflexive monitoring (reflection and appraisal).
This offers a useful way to consider how the challenges and enablers identified impacted on occupational therapists in this study.
Attitudinal challenges and enablers
Occupational therapists were required to change their practice by implementing COTiD, a new intervention, and adhering to VALID research procedures. Consistent with previous research, most described this as challenging, despite contrasting opinions about the intervention and research involvement ( Damschroder et al., 2009 ; Eriksson et al., 2013 ; May and Finch, 2009 ). Normalisation process theory explains that changes to practice are more likely to be adopted and viewed positively when individuals have coherence with them, i.e. new processes make sense to them ( May and Finch, 2009 ). Coherence varied between occupational therapists, perhaps in relation to how similar COTiD and the research procedures were to their usual practice, therefore how large the changes were, and how much they approved of the changes. For instance, some who usually provided short-term or more prescriptive interventions appeared to relish the opportunity to work in a more person-centred way, while others did not. Occupational therapists who appeared to have coherence with the research and intervention spoke positively about being involved in VALID, consistent with previous findings that positive attitudes towards research facilitate engagement ( Eriksson et al., 2013 ; Pain et al., 2015 ; Pighills et al, 2013 ; White et al, 2013 ).
Practical challenges
Occupational therapists reported being challenged by recruitment, overwhelming paperwork and using videos. Recruiting service user participants was described as time consuming and challenging, consistent with previous findings ( Hysong et al., 2013 ; Newall et al., 2009 ; Newington and Metcalfe, 2014 ). The importance of recruiting research participants to coincide with the readiness of therapists to work with them has been reported previously ( Gitlin et al., 2010 ), and this current study highlights the potentially negative impact on therapists’ motivation when it does not happen in a timely manner. Using videos and completing research paperwork presented challenges for many reasons, varying between occupational therapists. These included familiarity and confidence with using videos, organising and completing paperwork, compatibility of data transfer with organisational systems and occupational therapists’ and service users’ attitudes to being videoed. Learning new skills has often been described as challenging to research involvement, although usually with reference to research skills ( Akerjordet et al., 2012 ; McMaster et al., 2013 ; Pain et al., 2015 ), although problems using software have also been described previously ( Damschroder et al., 2009 ). Cognitive participation may have influenced the impact of these challenges, in that some occupational therapists who were more personally motivated to engage in the research were perhaps happier to invest more time and energy into learning the necessary skills and processes. Conversely, it may also be that occupational therapists who encountered fewer challenges more quickly gained coherence and this facilitated cognitive participation with the research.
Peer and management support and protected time were identified as enablers, reducing the impact of challenges, consistent with previous findings ( Eriksson et al., 2013 ; McMaster et al., 2013 ; Pain et al., 2015 ; Pighills et al., 2013 ; White et al., 2013 ). The mechanisms by which peer support enables research involvement have not previously been well described, but concur with previous reports that it is valued ( Eriksson et al., 2013 ; Gitlin et al., 2010 ). This study’s findings suggest peer support enables research involvement by increasing confidence through creating a safe environment for practising clinical skills, sharing thoughts and feelings about research engagement and clarifying research expectations.
Management support was identified as a key multifaceted enabler, consistent with previous research ( Newall et al., 2009 ; Pain et al., 2015 ; Perry et al., 2008; Pighills et al., 2013 ) . Management support provided: permission and encouragement for research involvement; assistance in negotiating with information technology departments to resolve software and hardware difficulties; support to negotiate with team members expressing negative attitudes towards research involvement; links to research and development departments to assist with recruitment and paperwork; and in some cases negotiating protected time for occupational therapists to engage in research. Protected time, with reduced clinical caseloads or time away from a usual clinical base, appeared an effective way to minimise clinical pressures, meaning that responding to crises was less likely to take priority over research activity, consistent with previous findings ( Newall et al., 2009 ). When occupational therapists had more time allocated to their VALID work they used it to learn the new intervention and attend to paperwork, therefore diminishing the impact of these challenges, which may have positively affected their attitude to research. Normalisation process theory explains these enablers through collective action as organisations demonstrated their support for research involvement, minimised additional burdens on occupational therapists and positively influenced their sense of coherence and cognitive participation with the research. The impact of reflexive monitoring was less evident, perhaps due to the relatively short-term nature of therapists’ research involvement or because occupational therapists engaged in reflective monitoring within the focus groups.
Implications
The consistency with which enablers and challenges to research are reported suggests they can be pre-empted but that their impact will vary between organisations and individuals. Therefore, while engaging clinicians in research is challenging, research programmes should try to ensure participating clinicians have access to protected research time, peer and management support. Positive attitudes to research should be encouraged and additional research tasks, such as recruiting participants, videoing and paperwork should be minimised. A greater understanding of the individual and organisational contexts in which occupational therapists work is required to assess the likely impact of challenges and enablers. It is, therefore, important to engage all stakeholders, service users, clinicians and managers, during the research planning phase to identify and minimise challenges and maximise the use of enablers ( Eriksson et al., 2013 ; May and Finch, 2009 ). As well as helping practically, doing so may help to foster collective action, increase coherence and cognitive participation with the research, thus increasing the probability of successful implementation.
More in-depth study of enablers and challenges to delivering interventions as part of research studies would be beneficial to increase understanding about their impact, how they interact and vary between professional groups, organisational contexts or research designs. This could be achieved by using methods which gather more in-depth data, or data from a greater number or wider variety of participants. For instance, the themes arising in this study could be used as the basis for wider investigation such as through a quantitative semistructured survey or qualitative interviews.
VALID research programme’s response to identified challenges and enablers
In the next stages of the VALID programme a number of steps were taken to enable occupational therapists’ research involvement. These included replacing video recording the intervention sessions with audio recording, minimising amendments to research paperwork and procedures, and allocating more time to practising use of hardware and software and related procedures within the training. Also, managers were invited to attend the training so as to understand better the requirements, dedicated research staff took responsibility for recruiting and consenting research participants and pre-trial checks were completed to guide research sites towards facilitating clinician involvement. Future publications will report on the impact of these changes.
Limitations
As a focus group study it is not possible to generalise from these findings. It is not known whether these findings reflect the views of the other occupational therapists who participated in the VALID research programme but declined to participate in the focus groups, or whether they are representative of other occupational therapists with similar research experiences. As the focus groups were multipurpose, they may not have captured the full extent of opinions on research involvement. Finally, because transcription was outsourced it was not possible to be confident in ascribing quotations to individual participants.
This study identified that while involving occupational therapists in research is challenging, it can be enabled by providing support, protected time and encouraging positive attitudes. While specific challenges and enablers were highlighted, which were broadly consistent with previous research, the need to consider them within individual and organisational contexts was also highlighted. Therefore, to enable occupational therapists’ involvement in research, multifaceted collective action involving all stakeholders is required to minimise challenges and maximise enablers. It is important to overcome challenges to research involvement so that occupational therapists can contribute to research alongside clinical practice, in line with their code of ethics and professional practice ( College of Occupational Therapists, 2015 ). Also, to demonstrate the clinical effectiveness of their interventions, increase the occupational therapy evidence base and improve outcomes and experiences for service users.
Key findings
Occupational therapists’ research involvement is challenged by implementing research tasks and new interventions but enabled by support, protected time and positive attitudes. Contexts vary the impact of challenges and enablers.
What the study has added
This study has increased understanding of the challenges and enablers of engaging occupational therapists in research, through delivering interventions within research studies.
Acknowledgements
The VALID research team would like to thank the occupational therapists who took part in the focus groups. The VALID research team acknowledge the support of the National Institute for Health Research Clinical Research Network.
Research ethics
Ethical approval was obtained from the Yorkshire and the Humber – Leeds West National Health Service (NHS) Ethics Committee (reference number 12/YH/0492) on 16 November 2012. The study was also granted NHS research and development approval (reference number 13762). All participants provided written informed consent.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article:This manuscript presents independent research funded by the National Institute for Health Research’s Programme Grants for Applied Research Programme (RP-PG-0610-10108). The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health.

61 Best Occupational Therapy Research Topics
Occupational therapists help people of all ages to recover and improve their physical, sensory, and cognitive activities. More than half of occupational therapists work in hospitals, while others work in nursing homes, educational facilities, and homes. But what does it take to be an occupational therapist? It would be best to study occupational therapy primarily up to the master’s level . Students are assigned projects as part of their course work through the studies. That is why we have selected the best occupational therapy research topics for your next assignment.
In occupational therapy, students always have trouble handling research projects. If you study occupational therapy and feel like you need help selecting a research topic, do not hesitate to contact us. Our writers go the extra mile and assist you in writing a top-notch research paper.
Do You Need Help in Selecting an Occupational Therapy Research Topic?
When you search “occupational therapy research topics, “it is not easy to trust platforms that offer academic consultation services. However, we offer expert writing services and professional research tips to keep your data confidential when you order from us.
Need help doing your assignment?
Often, occupational therapy students have a large workload which prevents them from doing every task on time. And when you have limited time, it becomes challenging to select a research topic.
We hope the tips below help you in your subsequent research:
1. Select a topic that interests you
When you select a topic that interests you, the research process becomes fun and engaging.
2. Narrow your topic
If your topic is too broad, it loses focus. Therefore, you should narrow down your scope to cover all the relevant information on the topic.
3. Review your research guidelines
Make sure that the research topic meets the requirements. If some of the guidelines are unclear, you should consult your professor or HelpForHomework to explain .
4. Read your class notes and do background research
Reading your notes helps in doing background checks on a topic. Knowing more about your research topic helps you develop a compelling argument for your paper.
5. Consider your audience
You should select a topic that is understandable to your audience. The research depends on your level of education as more comprehensive reports are high in the educational spectrum. Further, by identifying your audience, you can arrange details, tone, and supporting information in an appropriate presentation .
6. Create questions to evaluate your research topic
After finding a research topic, create questions to evaluate it. For example:
- Is the research feasible?
- How attractive is the research topic?
- What has been researched?
- What is the problem to be solved?
- What is the solution to the problem?
- How is your solution a good one?
- Who is the audience?
Qualities of an Excellent Occasional Therapy Research Topic
As we have recommended, always narrow down to a topic that interests you. After selecting a topic, you should check if it has the following qualities:
Clarity: Your occupational therapy research topic should be straightforward and understandable to your audience.
Complex: Your project topics should not be answerable by yes or no. The topic should be arguable and analytical.
Focused : Once you select a topic, check if it is narrow and focused and answer it thoroughly.
Your final research grade depends on how effective your topic selection is. It would be best if you prepared for your research early. However, if you need help, do not hesitate to contact us. But first, go through the occupational therapy research topics below and tell us what you think.
Hot Occupational Therapy Research Topics
Hot occupational therapy research topics should help you in creating a unique project. Before selecting a topic, you should examine the aspects that are preferable to you and what interests you the most. But it would be best if you did not worry as we have a list of top recommendations to save you .
- Discuss the progress made in a decade in occupational therapy for adults
- Ethics in occupational therapy
- Explain the role of occupational therapy for patients with stroke
- How do diabetic patients benefit from occupational therapy?
- How does culture affect occupational therapy?
- How is occupational therapy important in controlling dementia?
- How is occupational therapy necessary in pain management?
- Is occupational therapy truly occupational?
- Occupational therapy for breast cancer patients
- Occupational therapy in disease prevention
- Role of occupational therapy in disaster preparedness and management
- Role of occupational therapy in functional literacy
- Role of occupational therapy in the management of depression
- Role of occupational therapy in the management of eating disorders
- What is the role of occupational therapy in schools?
Good research topics for occupational therapy
An excellent occupational therapy research topic should be comprehensive and enjoyable to read. When formulating a research topic, you should ensure that you are original, specific, and concrete. We hope you find the best research topic from the list below:
- Benefits of occupational therapy for adult mental health patients
- Between bottom-up and top-down approaches, which method is effective for patients suffering from a stroke?
- Coexistence between teachers and occupational therapists in a school setting
- Discuss the stereotypes in occupational therapy practice
- Evaluate occupational therapy for patients with a brain tumor
- How can occupational therapy be used to prevent human trafficking?
- Interventions used by occupational therapists when treating spinal cord injuries
- Occupational therapy for cancer patients with metastatic disease
- Occupational therapy for inpatient
- Occupational therapy for terminally ill patients
- Occupational therapy in mental health management
- Role of occupational therapy in symptoms control
- The role of occupational therapy for prisoners
- The use of apps in occupational therapy treatment
- What are the therapeutic outcomes of occupational therapy?
Occupational therapy student research topics
It may seem challenging to select the best occupational therapy research topic, so the trick is to narrow down and select one that fascinates you. Always take your time, research a list of topics, and choose the one you can support. Here are some of the topics to consider:
- Critical historical analysis of occupational therapy
- Does occupational therapy affect politics
- Foundations of occupational therapy practice
- Impact of the gender of providing occupational therapy services
- Importance of occupational therapy in school mental health
- Leadership in occupational therapy
- Occupational therapy for children with autism
- Occupational therapy for people who have hip replacement
- Occupational therapy models for families
- Role of occupational therapy for children with sensory modulation disorder
- Role of occupational therapy in managing sleep
- Role of occupational therapy in psychiatry
- Scope of occupational therapy
- Students perception of occupational therapy
- Teacher’s perception towards occupational therapy
- The perspective of sensory integration approach in occupational therapy
Pediatric occupational therapy research topics
Pediatric occupational therapists seek to understand children’s motor skills, cognitive abilities, and social development. The therapists also check factors that may hinder children’s growth or ability to perform certain tasks at a specific age.
While studying pediatric occupational therapy, students go through a hassle in selecting a research topic. That is why HelpForHomework compiled the best 15 Pediatric occupational therapy research topics for you.
- A profile of your country pediatric occupational therapy
- Competency of a pediatric occupational therapist in the USA
- Correlation between obesity and academic achievement
- Discuss how religion and culture affect decision making in pediatric occupational therapy
- Effects of COVID-19 to outpatient occupational therapy
- How effective are the weighted vests in pediatric occupational therapy?
- How effective is the standing frame to children with cerebral palsy?
- Policies governing pediatric occupational therapy
- Risk factors correlating with musculoskeletal complaints from children
- The role of pediatric occupational therapy to children with osteosarcoma
- Treatment methods of lower limb spasticity in children with cerebral palsy
- Treatment of neonatal jaundice
- Use of video occupational therapy modeling for children
- What is the role of pediatric occupational therapy?
- What is your perspective on occupational-based pediatric therapy?
Need Help With Occupational Therapy Research?
Now that you have an occupational therapy research topic, do you need help in writing? Our support department is on standby to help you get top-quality expert papers. Further, if you need more clarification on project topics, do not hesitate to contact us. We assure you of personalized and professional help whenever you consult us for your assignments. Also check out Physical Therapy Research Topics .
Recent Posts
- The Role of Peer Reviews in Enhancing Your Graduate Essays
- Do You Say Masters or Master’s?
- Writing A Case Conceptualization
- Degree Accelerator Guide: Fast-Track Your College Education
- Care Plan Approaches
You cannot copy content of this page
Attention: UniSA network-related systems are currently down - impacting internet access and access to resources.
Phone support is available on 1300 137 659
Develop your research question
- Search for your assignment
- Find books and journal articles
- Find government and organisation information
- Forgotten Australians
- Children and Youth
- Finding resources for your assignment
- REHB 6006: OT Field Practice 4: Critical Appraisal Topic
- Evidence-Based Practice
STEP 1: Understand your research objective
Before you start developing your research question, think about your research objectives:
- What are you trying to do? (compare, analyse)
- What do you need to know about the topic?
- What type of research are you doing?
- What types of information/studies do you need? (e.g. randomised controlled trial, case study, guideline, protocol?)
- Does the information need to be current?
Watch the following video (6:26) to get you started:
Key points from the video
- All good academic research starts with a research question.
- A research question is an actual question you want to answer about a particular topic.
- Developing a question helps you focus on an aspect of your topic, which will streamline your research and writing.
- Pick a topic you are interested in.
- Narrow the topic to a particular aspect.
- Brainstorm some questions around your topic aspect.
- Select a question to work with.
- Focus the question by making it more specific. Make sure your question clearly states who, what, when, where, and why.
- A good research question focuses on one issue only and requires analysis.
- Your search for information should be directed by your research question.
- Your thesis or hypothesis should be a direct answer to your research question, summarised into one sentence.
STEP 2: Search before you research
The benefits of doing a background search :
- You can gather more background knowledge on a subject
- explore different aspects of your topic
- identify additional keywords and terminology
| : You can do at any stage of the development of your question. |
STEP 3: Choose a topic

| In this step, a will help you identify articles and books which can inspire more ideas and reveal aspects of your research interest that you may not have considered. |
The resources linked below are a good place to start:
- UpToDate It covers thousands of clinical topics grouped into specialties with links to articles, drugs and drug interaction databases, medical calculators and guidelines.
- An@tomedia This online anatomy resource features images, videos, and slides together with interactive, educational text and quiz questions.
- Anatomy.tv Find 3D anatomical images; functional anatomy animations and videos, and MRI, anatomy, and clinical slides. Test your knowledge through interactive activities and quizzes.
STEP 4: Brainstorm your questions
Now you have explored different aspects of your topic, you may construct more focused questions (you can create a few questions and pick one later).

| A will show you how others formulate their questions, hence expand your research direction. |
Learn more:
- Clear and present questions: formulating questions for evidence based practice (Booth 2006) This article provides an overview of thinking in relation to the theory and practice of formulating answerable research questions.
STEP 5: Pick a question and focus
Once you have a few questions to choose from, pick one and refine it even further.

| A may help you identify additional keywords in this step. |
Are you required to use "PICO"?
- PICO worksheet
- Other frameworks
The PICO framework (or other variations) can be useful for developing an answerable clinical question.
The example question used in this guide is a PICO question: How does speech therapy compare to cognitive behavioural therapy in improving speech fluency in adolescents?
| OR | teenager with a stutter | |
| | speech therapy | |
| | cognitive behavioural therapy | |
| | speech fluency |
| : PICO is one option, there are other frameworks you can use too! |
Use the interactive PICO worksheet to get started with your question, or you can download the worksheet document.
- Building your question with PICO
Here are some different frameworks you may want to use:
| opulation ( atient), ntervention, omparison ( ontrol) and utcome. Add a imeframe if required. Used particularly for treatment type questions. | |
| A variation of PICO where = xposure and = imeframe if required. | |
| Developed in the context of practice guideline adaptation. Includes = rofessionals/ atients, = utcome and = ealthcare Setting. | |
| = etting (where), = erspective (for whom), = ntervention (what), = omparison (compared with what), = valuation (Booth 2006). | |
| = ample, = henomenon of interest, = esign, = valuation, = esearch type. Useful for qualitative or mixed method studies (Cooke, Smith and Booth 2012). | |
| = Expectations, = lient group, = ocation, = Impact, = rofession, = ervice (Wildridge & Bell 2002). | |
| = Political, = Economic, = ocial, = echnological, = nvironmental, = egal (CIPD 2010). |
There are a number of PICO variations which can be used for different types of questions, such as qualitative, and background and foreground questions. Visit the Evidence-Based Practice (EBP) Guide to learn more:
- Evidence Based Practice guide
- << Previous: Plan your search
- Next: Search for your assignment >>
- Last Updated: Jul 4, 2024 11:22 AM
- URL: https://guides.library.unisa.edu.au/OccupationalTherapy
The text within this Guide is licensed CC BY 4.0 . Image licenses can be found within the image attributions document on the last page of the Guide. Ask the Library for information about reuse rights for other content within this Guide.
- Staff intranet
- Student intranet

What do you want to do?
Occupational therapy research projects, our research active academics are developing or furthering knowledge in occupational therapy which can be implemented into practice or education..
Below are some examples of the ground-breaking projects our academics have completed or are currently working on:
Total number of results: 44

Physical activity and sedentary behaviour in Fabry disease

Parenting across cultures in contemporary England

Writing in the digital age: Keyboard versus pen in adolescents
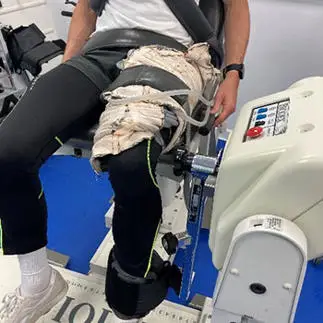
Understanding the role of temperature on muscle function in older adults

Functional trajectories of people with chronic critical illness

Can SmartSocks™ help deliver care to people with dementia living in care homes?
Individual-level stroke risk prediction after risperidone treatment in dementia
Developmental coordination disorder

Physical activity and McArdle disease

When reading misfires: the case for letter confusability

Protect mental health COVID-19 study

Using mindfulness to reduce schizophrenia vulnerability
Occupational Therapy and Rehabilitation Sciences
- Defining the Research Question(s)
- Reference Resources
- Evidence Summaries & Clinical Guidelines
- Health Data & Statistics
- Patient & Consumer Facing Materials
- Images/Streaming Video
- Database Tutorials
- Crafting a Search
- Narrowing / Filtering a Search
- Expanding a Search
- Cited Reference Searching
- Find Grey Literature
- Save Your Searches
- Cite and Manage Sources
- Critical Appraisal
- Different Types of Literature Reviews
- Conducting & Reporting Systematic Reviews
- Finding Systematic Reviews
- Tutorials & Tools for Literature Reviews
- Mobile Apps for Health
- Last Updated: Jul 9, 2024 6:57 PM
- URL: https://guides.nyu.edu/ot
- Research topics related to
50 Research topics related to Occupational Therapy

- November 28, 2022
- No comments
Are you looking for research topics related to Occupational Therapy? this page might help you come up with ideas. Research topics are subjects or issues researchers are interested in when conducting research. A well-defined research topic is the starting point of every successful research project. Choosing a topic is an ongoing process by which researchers explore, define, and refine their ideas.
Occupational Therapy is a profession that focuses on helping individuals achieve independence and improved quality of life through various forms of therapy and treatment. Occupational Therapy is an interesting program that helps people who have disabilities or difficulties in various areas of their life, such as physical, mental, or cognitive problems, to be as independent as possible and stay healthy.
Occupational Therapists teach patients skills , provide motivation, make changes to their environment, use technology and other resources to help them, and use physical treatments . The reason for researching topics related to Occupational Therapy is to find answers, support theories, find solutions to issues, and to increase overall understanding of the field.
Research topics related to Occupational Therapy are areas of study that aim to enhance the understanding of the field and its practices. These topics can range from the effectiveness of different treatment methods to the impact of Occupational Therapy on the lives of those receiving it. By exploring these research topics, the goal is to advance the field of Occupational Therapy and provide even better outcomes for patients.
There are many research topics related to Occupational Therapy, depending on your specialization and interests. The topics below are only for guides. We do not encourage writing on any of them because thousands of people visit this page also to get an idea of what topics to write on.
- A psychophysiology study of sensory processing in meditators
- Absence of child support and its impact on child care in [location]
- Air pollution, brain health, and well-being in [location]
- An assessment and outcome measure for children’s wheelchair basketball
- Analyzing the feeling of depression and the stigma about it.
- Assessment of injury risk factors and mechanisms in elite netball
- Benefits of occupational therapy for adult mental health patients
- Between bottom-up and top-down approaches, which method is effective for patients suffering from a stroke?
- Breathing muscle strength in healthy children
- Childhood maltreatment: emotional consequences and potential intervention
- Coexistence between teachers and occupational therapists in a school setting
- Creating digital stories to understand living with multimorbidity
- Decision-making in Gaelic football
- Developmental coordination disorder
- Discuss the stereotypes in occupational therapy practice
- Does homelessness create to influence the psychology of people?
- Effect of clinical depression on adolescent children.
- Evaluate occupational therapy for patients with a brain tumor
- Frequent incidents of displacement and its aggressive effect on street children.
- Functional trajectories of people with chronic critical illness
- Gender differences in multitasking
- Gestalt grouping and perceptual averaging to boost memory capacity
- Healthy living and lifestyle promotion amongst teenage girls
- How can occupational therapy be used to prevent human trafficking?
- Improving motor function in children with cerebral palsy
- Inclination towards committing suicide- Method to deal with the issue.
- Interventions used by occupational therapists when treating spinal cord injuries
- Is there a need for society to question the mental sickness stigma?
- Knowledge translation in children’s occupational therapy
- Managing the intrinsic PTSD in the lives of medical veterans.
- Occupational therapy for cancer patients with metastatic disease
- Occupational therapy for inpatient
- Occupational therapy for terminally ill patients
- Occupational therapy in mental health management
- Parenting across cultures in contemporary England
- Physical activity and McArdle disease
- Promoting social connections using happy-to-chat badges
- Protect mental health COVID-19 study
- Recovering a sense of smell and taste
- Rehabilitation using virtual gaming
- Rehabilitation via home-based gaming
- Respiratory physiology, human performance, and health
- Risk factors for cognitive decline in LGBT+ older people
- Road cycling behavior of young adults
- Role of occupational therapy in symptoms control
- The effects of sonification on motor imagery ability
- The impact of task complexity, cognitive load, and anxiety on driving
- The influence of continuous mobility in the lives of orphan toddlers.
- The role of occupational therapy for prisoners
- The significance of group therapy at foster homes.
- The social displacement of Autistic children.
- The use of apps in occupational therapy treatment
- Using mindfulness to reduce schizophrenia vulnerability
- Virtual reality for NHS staff wellbeing
- Visual and emotional processing in early Parkinson’s disease
- What are disability and the stigma enveloping it?
- What are the therapeutic outcomes of occupational therapy?
- When reading misfires: the case for letter confusability
- Writing in the digital age: Keyboard versus pen in adolescents
Related Choice
Leave a reply cancel reply.
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
You May Also Like
70 research topics related to media.
- November 29, 2022
Research topics related to Social Media
- January 5, 2023
63 Research topics related to International Business
- November 26, 2022
51 Research topics related to Pharmacy
88 research topics related to management, 76 research topics related to nutrition.

You are here
- Practice resources

Top 10 priorities for occupational therapy research in the UK
Setting the research agenda for occupational therapy and addressing the unanswered questions that matter most to people accessing and delivering occupational therapy services.
The top 10 priorities for occupational therapy research in the UK have now been identified. Read the full report here
- How does occupational therapy make a difference and have impact on everyday lives?
- How can occupational therapists ensure that person-centred practice is central to how they work?
- How can occupational therapists work more effectively with the family and carers of people who access services?
- What are the long-term benefits of occupational therapy intervention?
- What are the benefits or impact of occupational therapy in primary care settings? (e.g. services delivered by your local general practice surgery, community pharmacy, dental and optometry (eye health) services)
- How can occupational therapy services be more inclusive of both mental and physical health?
- What is the role of occupational therapy in supporting self-management? (e.g. helping people with illness to manage their health on a day-to-day basis)
- What is the role or impact of occupational therapy in reducing hospital admissions?
- How can occupational therapists work most effectively with other professionals to improve outcomes for people who access services? (e.g. multi-disciplinary teams, commissioners, community agencies)
- What is the cost-effectiveness of occupational therapy services?
Download the top 10 and more information about the research priorities.
- Top 10 priorities for occupational therapy in the UK (PDF, 132.96KB)
Watch Dr Jo Watson, RCOT Assistant Director – Education and Research, talk about why these priorities are so important for setting the future direction of research for occupational therapy in the UK.

Making a difference
These priorities will set the research agenda for occupational therapy in the future and help us focus on addressing the unanswered questions that matter the most to people who access and deliver occupational therapy services.
Our focus now is to encourage and support members to undertake and contribute to research that helps to answer the questions set out in the priorities. Funding available through the RCOT Research Foundation will be focused on supporting research that addresses the top 10. We will also be working to influence the opening up of external research funding opportunities.
Having this clear agenda for research takes RCOT a step closer to achieving its vision for research which is to have, within the next decade, a UK-wide culture that embraces engaging in and with research as every occupational therapist’s business embedded within the profession.
Research builds the evidence base underpinning occupational therapy and improves the experiences and outcomes for people accessing our services.
The Priority Setting Partnership
Throughout the project, RCOT’s focus has been to ensure that people who access occupational therapy, their carers, occupational therapists and other health and care professionals have been involved in every step. We were able to achieve this by partnering with the James Lind Alliance (JLA) in a Priority Setting Partnership (PSP) to follow the JLA’s well-respected and inclusive process.
The first stage of the process was to find out what unanswered questions people had about occupational therapy that research could answer. After checking that they truly were unanswered questions, people were then asked to prioritise these questions, first through shortlisting in a nationwide survey and finally through reaching agreement in a final prioritisation workshop.
Each priority is an overarching summary question within which there may be several questions to be answered by research. You can download the raw data behind each priority below and from the JLA website .
Key documents
These key documents provide background information underpinning the top 10, including the questions that were submitted in the first survey and used to create the 66 summary questions in the second survey.
- JLA Occupational Therapy PSP - Workshop outcome - All prioritised questions from workshop (05-Aug-20) (PDF, 227.97KB)
- Data management spreadsheet – workshop questions (PDF, 269.93KB)
- Data management spreadsheet – all questions (PDF, 500.49KB)
- PSP engagement summary
- Question verification form
Thank you to everyone who has helped us to identify the UK’s top 10 occupational therapy research priorities. Our particular thanks go to people who access occupational therapy services and their carers, as well as all our members and other health and care professionals who took part in our surveys and workshop.
Our PSP was overseen by a Steering Group and we would like to thank the group members and Katherine Cowan, Senior JLA Adviser, who chaired the Steering Group, for all their hard work and support throughout the project. We are very grateful to the James Lind Alliance (JLA) for partnering with us on this important work.
Thank you also to all our project partners and supporters who promoted our PSP to their networks and helped us hear from a broad range of people who access occupational therapy services.
You can find out more about our Steering Group and project partners and supporters below.
The process
Below is a brief overview of the process we undertook in identifying the top 10 research priorities for occupational therapy in the UK. You can find out more about the process on the JLA website .
1. We've created a steering group.
Made up of people who have accessed occupational therapy, their carers and occupational therapists, this group agrees the scope of the project, the plan of action and takes responsibility for the PSP.
- Membership of the steering group is listed at the bottom of this page.
2. We ran a survey.
We created a survey and asked people who access occupational therapy services, their carers, occupational therapists and others with an interest in occupational therapy to respond by posing questions they would like research to answer.
3. We summarised the responses.
With oversight from the steering group, our Information Specialist sorted all the responses and created summary questions, which form the longlist of questions.
4. We checked the evidence.
The longlist of summary questions was checked against existing research evidence to ensure they haven’t already been answered. Questions that have already been answered by research were removed.
5. We ran a second survey.
We asked people who access occupational therapy services, their carers, occupational therapists and others with an interest in occupational therapy to prioritise the questions in an interim priority setting survey. We are analysing the responses to create a shortlist of summary questions which will be discussed at a workshop on 27 July 2020.
6. We ran a workshop.
The prioritised summary questions from the interim priority setting survey will be discussed in an online one-day workshop on Monday 27 July 2020. People who access occupational therapy services, carers and occupational therapists will together agree the top 10 list of priorities. The workshop will be facilitated by advisers from the James Lind Alliance.
7. We published and are now promoting the top 10 research priorities.
The top 10 will be announced and published on the RCOT and JLA websites, promoted to researchers and research funders. The PSP will work with researchers and research funders to further develop the priorities into specific research questions.
Next steps for the Top10 research priorities
Identification of the Top 10 research priorities for occupational therapy in the UK is just the start of ongoing work.
What RCOT are doing to take the Top 10 research priorities forward?
- Distributing the full report widely, including to key research funders in health and social care, publication in a peer-reviewed journal, ongoing promotion via social media, the RCOT website and its newsletters and bulletins, conference and other presentations and workshops.
- Linking the Top 10 priorities to funding available to members through the RCOT Research Foundation.
- Expanding the range of resources and opportunities offered to develop members’ research-related confidence and skills.
- Lobbying for greater access to and uptake of practice-based research-related career pathways.
- Working with members of RCOT’s Specialist Sections to support them to identify research questions relevant to their own particular areas of specialist practice that help to address the Top 10.
- Supporting our Specialist Sections to engage meaningfully with people with lived experience, including those from under-represented and marginalised groups within society, to ensure they are involved the process of developing specific practice based research questions.
- Sharing questions submitted in the initial consultation survey related to influencing government policy and service provision but out of scope of the OTPSP with the RCOT Professional Practice team to help inform their policy and public affairs work and other campaign and promotional work.
- Sharing other out of scope questions submitted in the initial consultation survey and related to education of the public or occupational therapists themselves, career promotion, diversification of the workforce and raising the profile of the profession, with RCOT departments leading ongoing strands of work in those areas.
- Using the priorities to try to influence funding calls issued by external research funders in the health and social care environment.
- Monitoring the impact of the Top 10 through, for example, identifying funded research linked to the Top 10, its findings and impact on practice.
Getting involved in addressing the Top 10 research priorities.
The top 10 research priorities are broad summary questions. They were identified from a total of 66 summary questions derived from the 2000+ questions that were submitted to the PSP’s initial survey. Each of the top 10 questions provides an opportunity for several focused research questions to be generated across a range of service delivery contexts and areas of practice, across the lifespan and in relation to a whole range of different groups and communities.
- All occupational therapists regardless of their role or context of employment have a contribution to make to address the Top 10 priorities. Contributing to the development of the evidence base can support individual therapists to thrive and develop their careers, and a growing, robust evidence base will raise the profile of the profession.
- Departmental leads and service managers are encouraged to recognise and emphasise the inseparable relationship between engaging in and with research and the delivery of high-quality cost-effective practice. Building mutually advantageous partnerships with universities is a valuable approach that will not only help to answer those questions, but will also provide an opportunity to help build research capability and capacity within your team.
- Occupational therapists who are working towards developing their research-related skills and confidence are encouraged to contribute to identifying practice-related research questions that address the Top 10. It might be possible to work in partnership with those with more research experience and expertise to address those questions, and to help shape and inform study designs in partnership with those who access services. Seeking opportunities in a way that supports individual development and simultaneously supports a study to progress, for example through contributing to a literature review, helping to recruit participants or collecting data will contribute to addressing the top 10.
- Pre- and post-registration learners are encouraged to consider how the Top 10 might help to shape their individual research projects. Students and apprentices themselves can consider how their research project might make a small contribution. Maybe, over time, that idea might grow into a whole programme of research directed by one of the profession’s research leaders of the future.
- Occupational therapy academics are encouraged to incorporate reference to the Top 10 within pre- and post-registration education to help inspire and build the research-related knowledge, skills and confidence of the next generation of practitioners and researchers.
- Established researchers, whether employed in practice or academia, are encouraged to develop future programmes of research that actively address specific elements of the Top 10. Using the Top 10 priorities can support bids to highlight the value and importance of the research to funders. Building in opportunities for the research-related up-skilling of other occupational therapists will benefit the profession and professional practice.
We all have a role in contributing towards addressing the Top 10 priorities. The RCOT Research and Development Strategy (2019) highlights that doing so helps ensure that the individuals, groups and communities we work with receive the best possible input from the profession and that services are developed and delivered in the most cost-effective way. Your contribution to taking the Top 10 priorities forward can make a difference.
What is the James Lind Alliance and why has RCOT partnered with them on this project?
The James Lind Alliance is a non-profit making initiative established in 2004. Its infrastructure is funded by the National Institute for Health Research (NIHR). It brings patients, carers and clinicians together in Priority Setting Partnerships (PSPs) to identify and prioritise the top 10 unanswered questions or evidence uncertainties that they agree are the most important.
RCOT decided to work with the James Lind Alliance to make use of its high-profile, credible and well-established methodology which ensures that people with lived experience and people with professional expertise work in partnership to identify and agree the priorities that emerge from the process. RCOT’s Occupational Therapy Priority Setting Partnership project was launched in March 2019.
How were the members of the Steering Group selected?
An open call for expressions of interest to join the Steering Group was shared in OTnews , on the RCOT website, through RCOT newsletters and social media and via direct communications with a range of networks. RCOT used its existing connections with external organisations focused on Patient and Public Involvement (PPI) to publicise the open call for expressions of interest to people with experience of accessing occupational therapy and their carers/families.
32 expressions of interest were received from people with professional expertise and seven were received from people with experience of accessing occupational therapy and their carers/families. 13 people with professional expertise were invited to join the Steering Group, based on their area of expertise, the sector they work in, level of experience and their geographical location. Five people with experience of accessing occupational therapy services and their families/carers were invited to join the Steering Group based on a similar set of criteria.
The membership of the Steering Group is available further down this webpage.
What efforts were made to hear from a diverse range of people, including those from BAME backgrounds and other minority or marginalised groups, people with learning difficulties and older people?
Throughout the project we aimed to engage as wide an audience as possible, which also included reflecting the population across the UK as recorded in the 2011 UK Census.
Throughout the project, RCOT used the INVOLVE Guidelines to inform the way we work with people who access occupational therapy services and their carers/families. We enabled people’s participation by recompensing them for their time in preparing for and attending meetings, compensated them for their travel and any associated costs for personal assistants. Outside the core project team, 25% of the PSP Steering Group were people representing those who access services and their carers. Amongst them were the Deputy Chair of the National Co-Production Advisory Group and the Chair of the Think Local Act Personal Board.
We recognised that an online survey would not be accessible to everyone, so alternative ways of sharing and responding to the surveys were provided, including:
- An easy-read version of the first survey which was available to download from our website or offered as a hard copy on request.
- Downloadable resources on our website such as posters and flyers and hard copies of the survey (in Word and PDF). The project team was also able to send hard copies of survey materials along with a stamped addressed envelope.
- Welsh versions of both surveys were available online and to download (in Word and PDF).
- Communicate2U was a partner on the project and facilitated a discussion with their audience to ensure that people with learning disabilities had the opportunity to respond to the first survey.
- For the second survey, the project team ran an online facilitated discussion, in partnership with the National Co-production Advisory Group at Think Local Act Personal, to facilitate engagement with people with experience of accessing occupational therapy services and carers.
- A Steering Group member also conducted one-to-one discussions with seven men from ethnic minority populations to capture their responses to the second survey.
- A presentation by the project lead to occupational therapy students at the University of Cardiff in October 2019 to support and encourage students to respond to the first survey.
To help us connect with as wide an audience as possible, we developed a network of around 100 supporters to the project, including 50 partner organisations. These included individuals, charities and networks of people affected by particular conditions and those working with particular minority ethnic groups. The Race Equality Foundation and Sporting Equals UK are two examples of organisations that we asked to share the survey with their networks.
To monitor the diversity of respondents to the two surveys, we asked people to provide additional information on a voluntary basis. This included where in the UK people lived (for example, Scotland, Wales, Northern Ireland and England), age range, how people would describe their gender, ethnicity and whether they identified as disabled. The diversity of respondents was monitored throughout. Where it was identified that we wanted to hear from more individuals from a particular population, we sought the advice of our Steering Group members and approached individuals from relevant organisations and networks to try to help us increase awareness of and engagement with the surveys.
927 people responded to the first survey of which 2.48% of responses came from people who identified as Asian/Asian British, 0.76% of responses came from people who identified as Black/Black British, 0.32% of responses came from people who identified as Chinese or another ethnic group and 2.3% identified as mixed/multiple ethnicities.
Of the 1,140 responses to the second survey, the proportion of responses from the BAME community was similar to the first survey, with approximately 2% of responses from people who identified as Asian/Asian British, 2% who identified as Black/Black British and 1% who identified as mixed/multiple ethnicities.
The proportion of the UK population that identify as Asian/Asian British is 7.5%, Black/Black British 3.3% and Chinese or other ethnic group is 1%.
The final stage of the project was the final prioritisation workshop, where we specifically invited applications from people who:
- Have accessed occupational therapy
- Are aged over 65
- Are young adults (aged 16-24)
- Are family and carers of people who have accessed occupational therapy
- Are from Black and minority ethnic groups
- Are from a variety of social backgrounds
- Are occupational therapists working in frontline practice or leading and managing frontline services
Invitations were extended to ensure that the participants would represent the four nations of the UK, a range of practice areas and contexts, a range of professional experience, and a range of perspectives across the lifespan and in relation to a range of lived experiences of the impact of physical and mental health challenges.
What did RCOT learn from the experience of engaging with this wider audience, which included people with experience of accessing occupational therapy services and their carers/families?
We learnt that it is a challenge to build strong relationships with other organisations in a short period of time for a very specific objective. We need to build trust with these organisations and their communities, and this takes time. In discussion with the Race Equality Foundation, we learnt that the response from members of the communities they serve was likely to be low without face-to-face contact. We continually monitored the responses to the surveys to identify any gaps and developed our networks reactively through personal introductions to try to optimise the diversity of people responding to both surveys and expressing an interest in participating in the final prioritisation workshop.
We also learned that effectively engaging with people with the diversity of experience and backgrounds that reflects the diversity of individuals who access and deliver occupational therapy services can be challenging. Additionally, a commitment is needed to work with trusted individuals who are already working with particular communities.
How were the participants in the final prioritisation workshop selected?
An open call for expressions of interest to participate in the final prioritisation workshop was publicised in OTnews , on the RCOT website, through RCOT newsletters and social media and via direct communications with a range of networks. It was also promoted to and through external organisations focused on Patient and Public Involvement (PPI), such as the People in Research website, to raise awareness of the opportunity among people who access occupational therapy and their carers/families.
RCOT received 79 expressions of interest: 25 from people with experience of accessing occupational therapy services and their carers/families and 54 from occupational therapists. From these, 10 people with lived experience and 10 professionals were invited to participate in the final prioritisation workshop. Invitations were extended to ensure that the participants would represent the four nations of the UK, a range of practice areas and contexts, a range of professional experience, and a range of perspectives across the lifespan and in relation to a range of lived experiences of the impact of physical and mental health challenges.
How did COVID-19 affect the project?
The second initial prioritisation survey opened on 26 February 2020 and was due to close on 14 April 2020, ahead of a final prioritisation workshop that was initially planned for 1 June 2020. The implications of the global pandemic required that we postpone the final workshop until 27 July 2020. The project team and the Steering Group took the opportunity to extend the window for responses to the second survey until 20 May 2020.
The final prioritisation workshop was held virtually. This approach ensured that a wide range of people were able to safely participate and share their views in the facilitated discussions, despite the ongoing impact of the pandemic.
Is the top 10 still relevant in the context of COVID-19?
The top 10 research priorities remain relevant in the context of COVID-19. Each of the research priorities is broad and the focused research questions that will emerge from many of them can be applied to the impact of COVID-19 on society across the four nations of the UK. Whilst COVID-19 is a new disease, there are many healthcare challenges which remain constant and will continue to require the skills and experience of occupational therapists.
Why doesn’t the list of priorities include questions related to specific conditions, symptoms, interventions and so on?
The Occupational Therapy Priority Setting Partnership followed the James Lind Alliance methodology. We had a first survey, open from 5 August to 5 November 2019, to gather questions, which was widely publicised and open to everyone to complete. People were invited to submit their questions about occupational therapy, these questions were then checked to see if they were already answered and refined into 66 questions. The Steering Group worked to ensure that the final 66 questions were in scope, considered fairly and stayed true to the respondents’ questions.
The 66 questions were then shared online in a second survey, open from 26 February to 20 May 2020, and people were asked to identify up to ten that they considered most important for research to answer.
The ranking of the 66 questions by people with lived experience and of professionals was scrutinised by the Steering Group. The decision was made that the top ten from each group (people with lived experience and people with professional expertise) were to be taken to the final prioritisation workshop, two questions were selected by both groups, resulting in a shortlist of 18 questions. The workshop was held on 27 July 2020, where 20 participants (10 people with professional expertise and 10 people with lived experience) spent a day in facilitated discussions to agree the final top 10.
Full details of the JLA methodology are set out on the JLA website .
The new top 10 priorities provide us with a means of focusing the efforts of the profession on research that matters most to the people accessing and delivering occupational therapy services. In the context of a profession with such a broad scope of practice, the nature of the priorities is to our advantage. Each of the top 10 priorities can be considered as a summary question, reflecting the individual questions submitted during the initial survey. There will be several, more focused research questions that will need to be answered to address each of the priorities. This means that the priorities can be applied to a wide range of conditions, symptoms, interventions, areas and contexts of practice, and so on, and across the lifespan and with particular communities amongst the population in mind. In due course, the data that informed each summary question will be available to view on the JLA website.
What happens to the questions that are not included in the top 10?
The longlist of 66 questions will be published on this webpage and on the JLA website and will be available to researchers and research funders to view. Other PSPs , such as the Palliative and End of Life Care PSP, have seen a number of questions from their longlists receive funding for research.
What happens next to the research priorities?
Identifying the top 10 research priorities is just the start of the process; the next task is to work on them. RCOT will use the priorities to set the agenda for funding available to members through the RCOT Research Foundation, which will help to focus efforts on addressing the top 10. RCOT will also seek to influence the funding opportunities available from other health and care related research funders.
Will there be any publications where I can read more on the project?
RCOT will produce a final project report and will submit an academic paper for consideration for publication. We hope the final report will be available in winter 2020/21.
In the meantime, if you would like to read more about the project and methodology, you will find more information on this webpage or the JLA website .
Why do the research priorities apply to the UK and not internationally?
The Royal College of Occupational Therapists is the professional body for occupational therapists in the UK and funded the project to agree the top 10 priorities for occupational therapy research in the UK. The World Federation of Occupational Therapists (WFOT) has previously undertaken work to identify the research priorities for the profession from a global perspective. These are available on the WFOT website .
Video, podcast and articles
Watch our psp video.

Listen to our research priorities podcast
In this podcast we follow one research priority, from its setting right through to its clinical application.
Listen to this podcast on Soundcloud , Apple Podcasts , Stitcher , Spotify .
Read blogs and articles about the research priorities
|
(Isaac Samuels and Jenny Mac Donnell interview for the James Lind Alliance) |
|
(Ruth Unstead-Joss writing for the James Lind Alliance) |
|
(Jenny Mac Donnell writing for RCOT) |
|
(Alexander Smith writing on the British Geriatrics Society website) |
|
(Sarah Markham writing on the British Medical Journal website) |
- Creating a new research agenda for occupational therapists (OT News article) (PDF, 606.13KB)
Our project partners
Our project partners and supporters represent people who have experience of accessing occupational therapy services, their carers/families and health and care professionals.
Our project partners and supporters
| Activity Alliance |
| Age Cymru |
| Age NI |
| Alzheimer Scotland |
| Annabelle’s Challenge |
| Autistica |
| British Academy of Childhood Disability |
| British Geriatrics Society |
| Birmingham and Solihull Mental Health NHS Foundation Trust |
| Black Country Partnership NHS Foundation Trust |
| Cardiff University |
| Carers NI |
| Canterbury Christ Church University |
| The Christie NHS Foundation Trust |
| Communicate2U |
| Cumbria, Northumberland, Tyne and Wear NHS Foundation Trust |
| Dementia Carers Count |
| Devon Partnership NHS Trust |
| Edinburgh Napier University |
| Glasgow Caledonian University |
| Health and Care Research Wales |
| Healthwatch Southwark |
| Hull and East Yorkshire Hospitals NHS Trust |
| King’s College Hospital NHS Foundation Trust |
| Leeds Beckett University |
| Mersey Care NHS Foundation Trust |
| Midlands Partnership NHS Foundation Trust |
| Mental health Occupational Therapy Interventions & Outcomes research Network (MOTION) |
| Mersey Care NHS Foundation Trust |
| MND Association |
| Muscular Dystrophy UK |
| NHS Grampian |
| National Co-production Advisory Group |
| Norfolk and Norwich University Hospitals NHS Foundation Trust |
| North East and North Cumbria NMAHP Research Implementation Group |
| Nottinghamshire Healthcare NHS Foundation Trust |
| Occupational Therapy Advisory Forum for Wales |
| ORiENT: Occupational therapy Research and Evidence based-practice NeTwork - Wales |
| Royal National Hospital for Rheumatic Diseases |
| Royal United Hospitals Bath NHS Foundation Trust |
| Skills for Care |
| Sheffield Occupational Therapy Clinical Academics |
| Sheffield Teaching Hospital NHS Foundation Trust |
| South London and Maudsley NHS Foundation Trust |
| Southern Health NHS Foundation Trust |
| Spinal Injuries Association |
| Sporting Equals |
| Stroke Association |
| Tees Esk and Wear Valleys NHS Foundation Trust |
| University Hospitals of Morecombe Bay NHS Foundation Trust |
| University of East Anglia |
| University of Northampton |
| University of Southampton - School of Health Sciences |
| University of the West of England |
| UK Parkinson's Excellence Network |
| Wrexham Glyndwr University |
| Yorkshire Fatigue Clinic |
Steering Group members
Anne addison.
Anne currently works at Great Ormond Street Hospital as Joint Head of the Occupational Therapy service and as a Clinical Specialist Occupational Therapist in Neurodisability. She is also a member of the National Executive Committee for the Children, Young People and Families Specialist Section of the Royal College of Occupational Therapy.

Dr Maria Avantaggiato-Quinn
Dr Maria Avantaggiato-Quinn is Associate Allied Health Professional Director for Specialist Children’s Services at NTW FT and Principal Occupational Therapist. Previously an RCOT Council Member for England and Leadership Fellow of the Health Foundation, Maria represents service managers on the National Council for AHP Research and is also a carer.

Dr Mary Birken
Mary is an occupational therapist and has worked clinically in community and inpatient mental health services prior to moving to research. Her research interests are in community mental health occupational therapy.
Currently she is a Research Fellow and coordinator for the UKRI Loneliness and Social Isolation in Mental Health Research Network at University College London.

Dr Michael Clark
Michael is Associate Professorial Research Fellow in the PSSRU at the London School of Economics and Political Science. He is also Research Programme Manager of the NIHR School for Social Care Research. He is editor of the Journal of Long-term Care, was a member of the steering group for the Adult Social Work Research Priorities Setting Partnership, and was on the RCOT UKOTRF commissioning panel.

Katherine Cowan
Katherine is Senior Adviser to the James Lind Alliance (JLA) and is chair of the Occupational Therapy Priority Setting Partnership (PSP) Steering Group. She has been a key contributor to the development of the JLA method since 2008 and has chaired and advised almost 40 PSPs internationally.

Dr Edward Duncan
Edward is an Associate Professor in applied health research. He has worked clinically as an occupational therapist in a variety of mental health settings. Edward is the editor of two international occupational therapy textbooks. His current research focuses on the design, delivery, and testing of complex interventions in pre-hospital emergency care, in both the UK and sub-Saharan Africa.

Clenton Farquharson
Clenton Farquharson MBE has extensive knowledge of health and social care, and other social policy areas, particularly in relation to equality, diversity and co-production. Clenton is Chair of the Think Local Act Personal Board, a member of the Coalition for Collaborative Care Co-production Group and a Trustee of In Control. He is Director of the disabled people’s user led organisation, Community Navigator Services CIC, and acts as a Skills for Care Ambassador. Clenton is passionate about how we influence services to work together and to listen to the people who use the services.

Dr Naomi Gallant
Naomi is an occupational therapist with a specialist interest in dementia care and frailty. She is currently completing her doctoral research into improving mealtimes for people with dementia in the acute hospital setting. Naomi has worked in a variety of older persons care settings as an Occupational Therapist. Her current role is an Occupational Therapy Team Lead in a frailty rehabilitation unit for older people. This role includes improving the dementia pathway and research capacity within the service.

Amy Mary Rose Herring
Diagnosed during her teenage years with Asperger’s and Post Traumatic Stress Disorder, Amy has focussed her work on prevention and shortening the health and social inequalities gap.
Aged 21, Amy was recognised as one of the top 15 leaders within Work and Education on the UK’s inaugural Autism and Learning Disability Leaders list 2018.
She has a number of roles across the NHS in Sussex, NHS England and Chairs the Parliamentary Inquiry Panel of Children and Young People’s Rights in Mental Health.

Dr Jane Horne
Dr Jane Horne is an applied health and social care researcher with an interest in rehabilitation, primarily, older people and stroke. She has worked in research for 10 years with leading senior academics who are occupational therapists by profession. She is the Research and Development lead for the RCOT Specialist Section for Neurological Practice and worked clinically in the NHS prior to joining the University of Nottingham in 2009.

Dr Anne Johnson
Dr Anne Johnson is a Consultant Occupational Therapist for the NHS and Macmillan Professional, Joint Clinical Lead of the Bath Centre for Fatigue Services and a Senior Lecturer, University of the West of England, Bristol. Specialising in long-term conditions management with a particular interest in ensuring ‘patient voice’ is represented in services provided.

Jenny Mac Donnell
Jenny Mac Donnell is the Project Lead on the Occupational Therapy Priority Setting Partnership. She has extensive experience of working in professional membership organisations on multi-disciplinary and collaborative research projects.

Dr Sarah Markham
Sarah is a mental health service user and a keen supporter of the value of occupational therapy and of RCOT. She is also a Visiting Researcher in the Department of Biostatistics and Health Informatics, IoPPN, King's College London. Her academic background is in pure mathematics. She has also published research papers regarding clinical trials, computer science and psychiatry.

Vonnie McWilliams
Vonnie McWilliams is manager of the Design Innovation and Assisted Living Centre in Northern Ireland and is the chair of RCOT’s Northern Ireland Regional Group.
Vonnie has expert knowledge and experience in the fields of catastrophic injury, neurology, physical disability, learning disability, oncology, chronic fatigue syndrome and ME, respiratory, dementia, respiratory, orthopaedics, and general medical conditions. She works with individuals and their carers across education, the NHS, care management companies, medico-legal companies, solicitors firms and voluntary agencies. Vonnie has also been a Cognitive Behavioural Therapist for the last 10 years.

Dr Sally Payne
Dr Sally Payne is an occupational therapist and Professional Adviser at the Royal College of Occupational Therapists. She has worked in the NHS with children and young people for many years and has a range of clinical, research and management interests. Sally’s PhD explored the lived experience of teenagers with developmental coordination disorder/dyspraxia.

Stephanie Platt
Stephanie Platt is the Occupational Therapy Lead for Inpatient Mental Health Services in Stafford. She has worked in a wide variety of mental health settings over her career currently specialising in psychiatric intensive care.
Stephanie has recently completed a clinical academic internship through the NIHR and has commenced her MRes in Clinical Health Research. She is passionate about improving quality of life and outcomes for individuals experiencing mental health problems.

Dr Jenny Preston
Dr Jenny Preston MBE is a highly experienced Consultant Occupational Therapist and non-medical Clinical Lead for Neurological Rehabilitation. Jenny combines clinical practice, research, education and strategic leadership within her role. She is an applied health researcher with an interest in neurology and the impact on everyday life.
In Scotland, Jenny is a key member of the neurological community contributing to the Healthcare Improvement standards for Neurological Care and Support (2019) and is a member of the Government’s National Advisory Committee for Neurology Conditions.

Isaac Samuels
Isaac is a committed, community-minded individual who has worked within the third sector for many years, including local and national Government, with charities and the Think Local Act Personal initiative.
His primary focus lies in supporting a systematic approach to improving services for those who need them, ensuring communities' voices are embedded at every level through co-production.
Isaac has achieved considerable influence and success in reducing barriers faced by people with impairments and other seldom-heard groups, by exploring these issues in an open, honest, reflective and supportive way.

Alexander Smith
Alex is a Stroke Association Postgraduate Fellow based at the Division of Population Medicine, Cardiff University. He graduated as an occupational therapist from Cardiff University in 2011.
His research ranges across many aspects of post-stroke care, treatment and rehabilitation and is focused on how to understand the outcomes of care or treatment from a service user’s perspective. Within his fellowship role, he is investigating standardised patient-reported outcome measures (PROMs) and is trialling a method of making PROMs easier to complete for stroke survivors.

Michael Turner
Michael Turner is a disabled person and has spent most of his career working the disability field. This has included many research and development projects, with a particular emphasis on user involvement and co-production. He helped set up the Shaping Our Lives national network of service users and disabled people and spent eight years working on co-production at the Social Care Institute for Excellence.

Ruth Unstead-Joss
Ruth is the Project Coordinator of the Occupational Therapy Priority Setting Partnership. Ruth’s background is in managing projects in the international development sector. She has extensive experience of managing volunteers. She also volunteers in a personal capacity, as a lay representative for other health initiatives in the UK.

Dr Gill Ward
Dr Gillian Ward is the Research and Development Manager at the Royal College of Occupational Therapists. As an experienced researcher she has published in the area of enabling and assistive technologies for older adults.

Dr Jo Watson
As the Assistant Director – Education and Research at the Royal College of Occupational Therapists, Dr Jo Watson is responsible for leading and shaping the occupational therapy profession in the UK in terms of pre-registration education, continuing professional development, and the building of research capability and capacity to help expand the evidence-base underpinning professional practice. Jo is the strategic lead for the RCOT/JLA Priority Setting Partnership.

Dr Phillip Whitehead
Phillip Whitehead is Associate Professor of Occupational Therapy at Northumbria University at Newcastle. Phillip’s expertise lies in the field of community occupational therapy spanning health and social care domains; his practice background is in adult social care services. He is particularly interested in the development and evaluation of interventions to promote wellbeing and prevent or delay the use of other health and social care services. His current research focusses on housing adaptations, double-handed homecare and intermediate care.

- Steering Group - Terms of Reference - Occupational Therapy Priority Setting Partnership (May 2019) (PDF, 640.2KB)
- Protocol - Occupational Therapy Priority Setting Partnership (May 2019) (PDF, 845.67KB)
| Dr Gillian Ward | Research and Development Manager |
American Speech-Language-Hearing Association
- Certification
- Publications
- Continuing Education
- Practice Management
- Audiologists
- Speech-Language Pathologists
- Academic & Faculty
- Audiology & SLP Assistants
Medicare Issues 2025 Proposed Payment Policies for Outpatient Services
July 17, 2024
The Centers for Medicare & Medicaid Services (CMS) recently proposed changes to the 2025 Medicare Physician Fee Schedule (MPFS) —which establishes payment policies and rates for Part B (outpatient) services—that could negatively impact Medicare payment and access to care. The following information highlights key provisions impacting audiologists and SLPs, what ASHA Advocacy is doing or has done, and what ASHA members can do.
The Top Line
- CMS estimates a 2.8% payment cut but it could be as high as 9% because of multiple budget control mechanisms that Congress controls.
- Despite extensive ASHA advocacy, CMS opts not to add audiology and speech-language pathology related services to the permanent telehealth services list .
- Updates to the therapy plan of care certification requirements could reduce administrative burden for SLPs .
- Caregiver training services (CTS) see a policy update that will allow SLPs to obtain a patient’s verbal consent .
- CMS provides no updates regarding the audiology access (“AB modifier”) provision .
There are two proposed policies that ASHA does not support : payment cuts and not including our services in the permanent telehealth list . We need to use our collective voices to fight against the pending 2.8% reduction to Medicare Part B payments and for securing permanent telehealth authority. Consistent, powerful advocacy is critical through the end of 2024 to ensure CMS is implementing the Medicare benefit so that clinicians are appropriately paid for the services they provide and to avoid jeopardizing patient access to care. Congress must act to prevent further debilitating payment cuts and loss of telehealth privileges in 2025 .
Payment Rates
Conversion factor.
CMS uses an annual conversion factor (CF) to calculate MPFS payment rates. For 2025, CMS estimates that the CF will be $32.36, representing a 2.8% decrease from the $33.29 CF for 2024. Although CMS included a 0.05% positive budget neutrality adjustment, the proposed decrease in the CF is mostly due to expiration of the temporary 2.93% positive adjustment that Congress implemented to temporarily mitigate significant payment cuts in 2024.
CMS’s regulatory impact analysis (RIA) estimates that audiologists and SLPs will see a cumulative 0% change in payments based on the CF update and policy changes proposed for 2025. However, cumulative payment changes experienced by individual clinicians or practices will vary because actual payment depends on several factors, including the clinician’s location and the specific procedure codes billed.
ASHA is analyzing the proposed adjustments to professional work, practice expense, and liability insurance values for individual procedure codes to determine how the CF will affect national payment rates for audiology and speech-language pathology services.
Additional Payment Cuts
Medicare providers face other cuts known as sequestration (2% reduction) and statutory "Pay-As-You-Go", or PAYGO (4% reduction), due to laws that control federal spending. Although these specific cuts aren’t addressed in the MPFS, they could result in a total cut of almost 9% to overall Medicare payments when added to the CF reduction.
Congress has acted each year by passing legislation that reduced or eliminated some of these additional cuts and will need to do so again for 2025 payments .
Next Steps for ASHA: Annual reductions hurt our members and their patients, which is why we have strongly advocated against Medicare Part B payment cuts since they were first set to occur in 2021. This vicious cycle requires all of us to push against CMS on its proposed changes and lobby Congress to intervene and to stop the payment cuts. Thankfully, Congressional intervention has helped soften the blow of the cuts each year, but it’s not enough. Medicare providers will continue to face payment instability unless Congress acts to reform the Medicare payment system. ASHA is fully committed to continuing advocacy and collaboration with members of Congress, CMS, key decision makers, and allied professional organizations (whose providers are also impacted) to find short- and long-term solutions to address Medicare payment issues, including supporting H.R. 2474, the Strengthening Medicare for Patients and Providers Act .
What You Can Do: ASHA members can take action by urging their members of Congress to fully address the multiple sources of payment reductions, including by cosponsoring H.R. 2474, which would provide an annual inflationary payment update based on the Medicare Economic Index. Ask your colleagues and friends to do the same to support this important legislation.
Coding Updates
Although there are no new or revised procedure codes directly related to audiology or speech-language pathology services for 2025, SLPs should be aware of proposed updates to policies around the caregiver training services (CTS) codes.
Caregiver Training
Beginning in 2024, SLPs have been able to report caregiver training services (CTS) without the patient present when provided under an established, individualized, and patient-centered plan of care. The proposed rule includes refinements to the existing CTS policies.
Patient Consent
One criterion for CTS billing requires the SLP to receive consent from the patient (or their representative) to provide caregiver training without the patient present; however, CMS does not dictate the form or manner of obtaining and documenting this consent. The flexibility of this policy is important to ensure clinicians can obtain consent in a manner that reduces administrative burden and maintains access to care for patients. In the proposed rule, CMS includes important and helpful guidance to allow verbal consent from the patient or the patient’s representative . The verbal consent must be documented somewhere in the patient’s medical record, but CMS maintains the flexibility to allow clinicians and facilities to determine their own protocols for obtaining and documenting consent.
Telehealth List
CMS is proposing to add CTS to the authorized telehealth services list for 2025, but on a provisional basis. In 2024, CTS was not an eligible telehealth service. However, given that audiologists and SLPs may not be eligible to continue to provide telehealth services in 2025 without Congressional action, it is unclear how helpful this flexibility will be.
New Caregiver Training G-Codes for Primary Care Services
CMS is proposing a new set of Medicare-specific G-codes for caregiver training without the patient present in direct care strategies and techniques to support care for patients with ongoing conditions or illness and to reduce complications (including but not limited to techniques to prevent decubitus ulcer formation, wound dressing changes, and infection control). These are similar to the existing CTS codes available for SLPs and valued at the same rate. These G-codes are intended to be used in primary care services.
Next Steps for ASHA : ASHA will seek clarification on how the new Medicare specific G-codes for caregiver training may overlap with services described in the CTS codes used by SLPs. We will express support for verbal consent from the patient or patient’s representative.
ASHA Request to Add Services to the Authorized Telehealth List
The structure of the Medicare telehealth benefit is split between Congress and CMS.
| Determines the clinical specialties who are eligible telehealth providers | Determines which services are covered telehealth benefits |
CMS has an established process for reviewing requests from the public to add Current Procedural Terminology (CPT®) codes to the authorized telehealth services list on a permanent basis. This process requires that a letter, outlining the codes being requested for addition to the list along with research and evidence supporting their inclusion, be submitted to the Agency by February 10 of each year. CMS staff review these requests and outlines their determinations in each year’s proposed rule.
ASHA submitted a request [PDF] in February 2024 requesting that CMS permanently add audiology and speech-language pathology CPT codes that have been temporarily authorized telehealth services since March 2021. While audiologists and SLPs may not be authorized telehealth providers in 2025 without Congressional action, ASHA maintains that the development of a robust telehealth benefit is critically important to ensure continuity of care for Medicare beneficiaries by ensuring there is a benefit in place that can be more easily implemented when these clinicians are added.
Unfortunately, CMS stated that it would not add any CPT codes that currently have provisional approval to the authorized telehealth services list in 2025―including audiology and speech-language pathology services―until it has performed a “comprehensive analysis” of these services . This proposal does not align with the formalized approval process developed by CMS. It does not address the merits of the request ASHA submitted earlier this year. Further, CMS fails to define what a “comprehensive analysis” is or what it would entail making it challenging, at best, to respond to this proposal. It also fails to provide a rationale for why a “comprehensive analysis” is required and why its own formalized review criteria are insufficient to make a determination to add these services to the authorized telehealth services list.
Updated Telehealth Policies
CMS will continue to allow clinicians who are providing telehealth services to Medicare beneficiaries from their homes to use their business address on claims to protect their privacy and security. CMS also proposes to permanently allow two-way, real-time audio-only communication technology to qualify as a telehealth service furnished to a beneficiary in their home if the clinician is technically capable of using audio and video equipment that enables two-way, real-time interactive communication, but the patient is not capable of, or does not consent to, the use of video technology . To use this flexibility, clinicians in outpatient settings will be required to report modifier “93” (audio-only synchronous telemedicine service) on the claim to verify that these conditions have been met.
Next Steps for ASHA : We are dissatisfied with CMS’s decision to not include audiology and speech-language pathology services on its proposed list of approved CPT codes, despite our efforts to work within their processes. ASHA is committed to securing permanent authority for audiologists and SLPs to receive payment for services provided via telehealth at parity with payment for in-person services. We will also strongly oppose CMS’s inaction in our comments.
What You Can Do : Visit ASHA’s Take Action site to urge your members of Congress to advocate for permanent telehealth coverage under Medicare.
Updates to the Therapy Plan of Care Requirements
For 2025, CMS is proposing amendments to the certification of the plan of care regulations to reduce the administrative burden for therapists and physician/nonphysician practitioners (NPPs) . These changes, if finalized, would provide an exception to the physician/NPP signature requirement on the therapist-established treatment plan for purposes of the initial certification. This exception would apply in cases where a written order or referral from the patient’s physician/NPP is on file and the therapist has documented evidence that the treatment plan was transmitted to the physician/NPP within 30 days of the initial evaluation.
CMS is also soliciting comments on the need for a regulation addressing the amount of time during which the physician/NPP who has written an order for therapy services could make changes to the therapist-established treatment plan by contacting the therapist directly.
Next steps for ASHA : ASHA will comment in support of this change because it reduces administrative burden for SLPs and their physician colleagues.
Supervision of Therapy Assistants
For 2025, CMS proposes a regulatory change to allow for general supervision of physical therapist assistants (PTAs) and occupational therapy assistants (OTAs) by PTs in private practice (PTPPs) and OTs in private practice (OTPPs) for all applicable physical and occupational therapy services. At this time speech-language pathology assistants (SLPAs) are not recognized under federal law as qualified providers and, therefore, their services are not covered. Once we secure coverage, we will need to confirm this policy applies equally to SLPAs.
Telesupervision of “Incident To” Services
SLPs, PTs, and OTs are allowed to provide services “incident to” a physician with direct supervision. “Incident to” coverage policies state that the services of the therapist would be billed under the National Provider Identifier (NPI) of the supervising physician. Direct supervision is typically defined as in the office suite and immediately available to help if needed . This definition was relaxed during the COVID-19 public health emergency to allow for telesupervision―supervision via real-time audio and visual interactive telecommunications.
CMS is proposing to allow telesupervision through 2025 for physical and occupational therapy and speech-language pathology services. In addition, it proposes to allow for telesupervision on a permanent basis for any CPT code with a professional and technical component (PC/TC) status indicator of “5” and services described by CPT code 99211 (Office or other outpatient visit for the evaluation and management of an established patient that may not require the presence of a physician or other qualified health care professional). CPT codes primarily billed by SLPs do not have a PC/TC status indicator of “5,” which means that unless CMS makes additional changes through rulemaking for 2026, SLPs will not be eligible to be telesupervised after 2025 .
However, CMS proposes to add services to the telesupervision list at any time if they meet specified criteria including the services that are inherently lower risk. This includes services that 1) do not ordinarily require the presence of the billing practitioner, 2) do not require direction by the supervising practitioner to the same degree as other services furnished under direct supervision, and 3) are not services typically performed directly by the supervising practitioner.
Next steps for ASHA : ASHA believes speech-language pathology services meet this proposed criteria for permanent telesupervision and will urge CMS to finalize telesupervision on a permanent basis.
Quality Payment Program (QPP)
The QPP transitions Medicare payments away from a volume-based fee-for-service payment to a more value-based system of quality and outcomes-based reimbursement. The program includes Advanced Alternative Payment Models (APMs) and the Merit-Based Incentive Payment System (MIPS).
Alternative Payment Models (APMs)
Only a small percentage of audiologists and SLPs participate in the APM track. These clinicians typically work for larger health care systems and have the support of finance and administration departments to manage the complexity of such models. CMS proposals in this rule would add new quality measures and reward efforts to improve health equity . They also request information on higher risk/higher reward options. Audiologists and SLPs working for organizations participating in APMs can help their organizations earn incentive payments by engaging in quality improvement efforts .
APMs are designed to improve the patient experience by encouraging collaboration between providers, improving quality of care, and making services more affordable. APM participants receive payments that reward them for the value of—rather than the volume of—services provided. Value, in this context, is outcomes of the intervention as related to cost. Accountable Care Organizations (ACOs) are one type of APM that takes system-wide responsibility for the care of an individual across all their health care needs.
To incentivize ACOs to serve more beneficiaries from underserved communities CMS is proposing a Health Equity Benchmark Adjustment (HEBA) to be applied based on the number of beneficiaries they serve who are dually eligible or enrolled in the Medicare Part D Low-Income Subsidy (LIS).
CMS is proposing to require ACOs to report the APM Performance Pathway (APP) Plus Quality Measure Set . This would include the 6 measures currently in the APP quality measure set and incrementally incorporate the remaining 5 Adult Universal Foundation quality measures by the 2028 performance period/2030 payment year with preference for reporting electronically through electronic clinical quality measures (eCQMs).
New measures included in the APP Plus Quality Measure Set for Shared Savings Program ACOs that could involve audiologists and SLPs include:
- #479 Hospital-Wide, 30-day, All-Cause Unplanned Readmission (HWR) Rate for MIPS Eligible Clinician Groups beginning in PY 2025
- #487 Screening for Social Drivers of Health beginning in PY 2028
CMS is also proposing a calculation methodology to account for the impact of improper payments when reopening a payment determination to recoup payments they believe were not properly earned.
Finally, CMS is seeking additional details from ACOs and other interested parties about the tradeoffs associated with a new higher risk / reward option than the current ENHANCED track.
Learn more about APMs and value-based care on ASHA’s website.
Merit-Based Incentive Payment System (MIPS)
CMS continues to focus on the transition from MIPS to MIPS Value Pathways (MVPs) by proposing new MVPs related to ophthalmology, dermatology, gastroenterology, pulmonology, urology, and surgical care. They are consolidating the two neurology-focused MVPs into a single neurology MVP. They are also requesting information on challenges clinicians may face in adopting MVPs, data reporting for public health, and the use of Patient- Reported Outcome Measures (PROMs), Patient-Reported Outcome Performance Measures (PRO–PMs), and Consumer Assessment of Healthcare Providers and Systems (CAHPS) for MIPS Survey. ASHA members can participate in MVPs as members of larger health care systems but not as individuals or as private practices because the current structure of MVPs does not allow for effective nonphysician participation.
CMS proposes to revise their cost measure scoring methodology to assess clinician cost of care more appropriately in relation to national averages. At this time, ASHA members are not required to participate in the cost performance category as there are no cost measures specific to audiology and speech-language pathology care management across an episode.
There are no changes to the audiology specialty measure set for the 2025 performance/2027 payment year.
We are pleased that CMS is proposing to add five measures to the speech-language pathology specialty measure set for the 2025 performance/2027 payment year in response to a request from ASHA last year [PDF]. Those measures include:
- Dementia: Cognitive Assessment : Percentage of patients, regardless of age, with a diagnosis of dementia for whom an assessment of cognition is performed and the results reviewed at least once within a 12-month period.
- Dementia: Functional Status Assessment : Percentage of patients with dementia for whom an assessment of functional status was performed at least once in the last 12 months.
- Dementia: Safety Concern Screening and Follow-Up for Patients with Dementia : Percentage of patients with dementia or their caregiver(s) for whom there was a documented safety concerns screening in two domains of risk: (1) dangerousness to self or others and (2) environmental risks; and if safety concerns screening was positive in the last 12 months, there was documentation of mitigation recommendations, including but not limited to referral to other resources.
- Dementia: Education and Support of Caregivers for Patients with Dementia : Percentage of patients with dementia whose caregiver(s) were provided with education on dementia disease management and health behavior changes AND were referred to additional resources for support in the last 12 months.
- Amyotrophic Lateral Sclerosis (ALS) Patient Care Preferences : Percentage of patients diagnosed with ALS who were offered assistance in planning for end of life issues (e.g., advance directives, invasive ventilation, lawful physician-hastened death, hospice) or whose existing end of life plan was reviewed or updated at least once annually or more frequency as clinically indicated (i.e., rapid progression).
Clinicians continue to be excluded from mandatory MIPS participation if they have: 1) allowed charges for covered professional services less than or equal to $90,000, 2) furnished covered professional services to 200 or fewer Medicare Part B-enrolled individuals, or 3) furnished 200 or fewer covered professional services to Medicare Part B-enrolled individuals. Given these standards, ASHA estimates that less than 1% of its members are subject to MIPS.
Additional information on MIPS is available on ASHA’s website.
Next Steps for ASHA : ASHA will request CMS finalize its proposal to add 5 new measures to the speech-language pathology specialty measure set under MIPS.
Social Determinants of Health (SDOH)
SDOH describes “conditions in the environments where people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks” ( Healthy People 2030 ).
CMS is requesting information on several new health-related social needs services including Social Determinants of Health Risk Assessment (SDOH RA) (HCPCS code G0136) currently used by primary care physicians. They are interested in the types of auxiliary personnel that are not adequately captured in current coding and payment for these services. They are also interested in any related services that billing practitioners and auxiliary personnel perform to address SDOH that may not be captured in current codes.
Z codes (ICD-10-CM codes Z55-Z65) are used to document an individual’s SDOH data and come in nine broad categories of SDOH known to affect patients’ health outcomes (e.g., housing, psychosocial, literacy). CMS is requesting information on the current utilization of Z codes, as well as barriers and opportunities to their widespread use.
Next steps for ASHA : ASHA supports collecting SDOH information to ensure patient needs are being met when these factors impact their experience and outcomes of care. Additionally, this information could help ensure payment adequately considers the impact of SDOH on the cost of care.
Find out more about SDOH on ASHA’s website.
Medicare Targeted Manual Medical Review
CMS notes that the Bipartisan Budget Act of 2018 permanently repealed the hard caps on therapy services and permanently extended the targeted medical review process first applied in 2015. Therefore, Medicare beneficiaries can continue to receive medically necessary treatment with no arbitrary payment limitations. However, clinicians must append modifier “KX” when medically necessary services reach a monetary threshold, which changes annually. For 2025, CMS estimates the “KX” modifier threshold will be $2,410 for physical therapy and speech-language pathology services combined. This represents an $80 increase from the 2024 threshold amount of $2,330 . Find more information regarding the permanent repeal of the therapy cap and the current targeted medical review process on ASHA’s website .
What’s next?
ASHA will submit comments by the September 9 deadline. The final rule will likely be issued in early November with implementation on January 1, 2025. We will keep members informed on developments.
ASHA Resources
- 2024 Medicare outpatient payment rates
- Take Action to stop Medicare cuts
- Take Action to make audiology and speech-language pathology services delivered via telehealth permanent
- Medicare resources
Please contact ASHA’s health care and education policy team at [email protected].
- Advertising Disclaimer
- Advertise with us
ASHA Corporate Partners
- Become A Corporate Partner

The American Speech-Language-Hearing Association (ASHA) is the national professional, scientific, and credentialing association for 234,000 members, certificate holders, and affiliates who are audiologists; speech-language pathologists; speech, language, and hearing scientists; audiology and speech-language pathology assistants; and students.
- All ASHA Websites
- Work at ASHA
- Marketing Solutions
Information For
Get involved.
- ASHA Community
- Become a Mentor
- Become a Volunteer
- Special Interest Groups (SIGs)
Connect With ASHA
American Speech-Language-Hearing Association 2200 Research Blvd., Rockville, MD 20850 Members: 800-498-2071 Non-Member: 800-638-8255
MORE WAYS TO CONNECT
Media Resources
- Press Queries
Site Help | A–Z Topic Index | Privacy Statement | Terms of Use © 1997- American Speech-Language-Hearing Association

IMAGES
VIDEO
COMMENTS
The research proposal The experience of putting together a research project, whether ... going to research. Occupational therapy is very diverse and ... mean the decision-making is even harder! Aim to choose a topic that you could potentially research in practice in the future, if not during your pre-registration education. It is important to ...
Topics | The American Journal of Occupational Therapy | American Occupational Therapy Association Topics Start here to explore in depth the topics that matter to you. Advocacy Alzheimer's Disease and Dementia Arthritis Assessment Development and Testing Assistive Technology Attention Deficit Hyperactivity Disorder Autism/Autism Spectrum Disorder Cardiopulmonary Conditions Centennial Vision ...
HIGHLY RECOMMENDED TO VIEW: Okay, ignore the silly beginning, because this video is a great (and short!) overview on how to select a research topic that's manageable for your assignment.Nice tips on narrowing a huge topic by considering the angles of WHO, WHAT, WHERE, WHY, WHEN, or HOW. Also, tips to keep from making a topic too narrow. (See box on right "Narrowing your topic" for other examples.)
Each year to determine the most influential research for us to review we generated a list the 100 most influential OT-related journal articles from the past 5 yeras. We team up with a research librarian to make this happen. For our 2024 list, we searched the Scopus database for articles published from 2019-2023 that had " occupational therapy ...
Methodology. Ethics. The Introduction section of the research proposal should provide the reader with an overview of your research. You want to take the time to briefly explain why you selected your topic and why it is important to your field. You will then want to express what your research adds to the field and why it is important.
OT-Student-resource-the-research-proposal-March2016.pdf. We're RCOT, the Royal College of Occupational Therapists. We champion occupational therapy. We're here to help achieve life-changing breakthroughs - for our members, for the people they support and for society as a whole.
Occupational Therapy Research Agenda. ... Pathfinders are guides to information sources on specific topics often researched by occupational therapists and directs you to specific and reliable sources of information on a topic. ... Participants in each track will be assigned to mentored pods to discuss and critique draft research proposals ...
OTJR: Occupational Therapy Journal of Research is published quarterly by the American Occupational Therapy Foundation, Inc. This international peer-reviewed journal offers empirical and review articles to readers interested in factors of human … | View full journal description. This journal is a member of the Committee on Publication Ethics ...
Research enablers. Within the theme of research enablers were four subthemes, 'peer support', 'management support', 'protected time' and 'positive attitudes towards research'. Each subtheme was identified in every focus group, with occupational therapy participants initiating discussion of the topic. Peer support.
61 Best Occupational Therapy Research Topics. Occupational therapists help people of all ages to recover and improve their physical, sensory, and cognitive activities. More than half of occupational therapists work in hospitals, while others work in nursing homes, educational facilities, and homes. But what does it take to be an occupational ...
Three presentations launched the second day morning discourse: (a) Current Occupational Therapy Perspectives in Mental Health Practice and Research, 1 (b) Community Engagement and Independent Living for Adults with Mental Illness, 2 and (c) Cognition and Function in Daily Life Activities. 3 Afternoon presentations were made by the three program ...
STEP 3: Choose a topic. Pick an area of interest and explore its different aspects to identify a topic. In this step, a background search will help you identify articles and books which can inspire more ideas and reveal aspects of your research interest that you may not have considered. The resources linked below are a good place to start:
ply your research skills. This guide provides signposting to resources and information that may be helpful when developing a student/learner research proposal, including: choosing a topic, partici. ant recruitment and ethics. Remember though, it's important to follow the specific guidance given by your university to su.
Case study methodology is a comprehensive research approach with origins in the health and social sciences and is being increasingly applied as a mode of enquiry in qualitative research (Salminen, Harra, & Lautamo, 2006; Stake, 1995; Thomas, 2011; Yin, 2014).A case study methodology may be employed when there is a phenomenon of interest that is situated in a natural, real-life context, where ...
Our research active academics are developing or furthering knowledge in occupational therapy which can be implemented into practice or education. Below are some examples of the ground-breaking projects our academics have completed or are currently working on: Total number of results: 44.
Occupational Therapy and Rehabilitation Sciences Guide to locating OT and Rehabilitation research evidence in books, journal articles, databases, and on the web. Home
Sex as an ADL. There are many forms of sexual expression which include actions such as kissing, hugging, and intercourse. Sexual activity occurs across the adult lifespan and may be with an intimate partner or with oneself. Engagement is often a positive experience; however, occupational therapy practitioners must consider any negative or ...
Occupational therapy research has a long and varied history of involving patients, public, and communities in research as advi-sors, collaborators, and co-researchers. In Canada, funding agencies have expected patients and knowledge users to be research team members for more than a decade, as illustrated in initiatives like the Canadian ...
The significance of group therapy at foster homes. The social displacement of Autistic children. The use of apps in occupational therapy treatment. Using mindfulness to reduce schizophrenia vulnerability. Virtual reality for NHS staff wellbeing. Visual and emotional processing in early Parkinson's disease.
The research proposal The experience of putting together a research project, whether ... going to research. Occupational therapy is very diverse and ... mean the decision-making is even harder! Aim to choose a topic that you could potentially research in practice in the future, if not during your pre-registration education. It is important to ...
Review of Occupational Therapy Research in the Practice Area of Children and Youth. PubMed Central. Bendixen, Roxanna M.; Kreider, Consuelo M. 2011-01-01. A systematic review was conducted focusing on articles in the Occupational Therapy (OT) practice category of Childhood and Youth (C&Y) published in the American Journal of Occupational Therapy (AJOT) over the two-year period of 2009-2010.
The Royal College of Occupational Therapists' research and development strategy 2019-2024 is intended to inform, guide and direct the development of research capability and capacity in the occupational therapy profession in the UK and the quality and impact of the associated research outputs. It builds on the research and development ...
People who access occupational therapy services, carers and occupational therapists will together agree the top 10 list of priorities. The workshop will be facilitated by advisers from the James Lind Alliance. 7. We published and are now promoting the top 10 research priorities.
This proposal does not align with the formalized approval process developed by CMS. It does not address the merits of the request ASHA submitted earlier this year. ... CMS is proposing to allow telesupervision through 2025 for physical and occupational therapy and speech-language pathology services. ... 2200 Research Blvd., Rockville, MD 20850 ...